Category - Part 5
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission: Response to Bronchodilators
 In asthmatics “in remission,” improvement in FEVi following bronchodilator was small although larger than in controls, with a percent change from baseline values ranging from —1.1 to 14.1 percent; mean, 5.7 ±0.8 percent (controls: —4.4 to 10.5 percent; mean, 2.5 ±0.6 percent; p=0.004). After 200 fig of inhaled albuterol, FEF25-75% increased 2.2 to 50 percent from baseline; mean, 17.3 ±2.6 percent) (controls: —4.3 to 39.8 percent; mean, 13.5±2.3 percent; NS). The increase in FEF25-75% was the sole parameter that was statistically different when the five hyperreactive control subjects were either kept in the control group or replaced: mean response with hyperreactive subjects replaced was 11.5 ±1.9, p=0.024).
In asthmatics “in remission,” improvement in FEVi following bronchodilator was small although larger than in controls, with a percent change from baseline values ranging from —1.1 to 14.1 percent; mean, 5.7 ±0.8 percent (controls: —4.4 to 10.5 percent; mean, 2.5 ±0.6 percent; p=0.004). After 200 fig of inhaled albuterol, FEF25-75% increased 2.2 to 50 percent from baseline; mean, 17.3 ±2.6 percent) (controls: —4.3 to 39.8 percent; mean, 13.5±2.3 percent; NS). The increase in FEF25-75% was the sole parameter that was statistically different when the five hyperreactive control subjects were either kept in the control group or replaced: mean response with hyperreactive subjects replaced was 11.5 ±1.9, p=0.024).
Continue reading this post…
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission: Results
Results were similar whether the five hyperreactive subjects were replaced or not, except for bronchodilator response, as commented in this section. Therefore, the results presented are those of the 30 ex-asthmatics in comparison to the 30 initial controls, including these 5 hyperreactive subjects.
Our subjects reported no symptom attributed to asthma or any need for antiasthma medication for periods of 2 to 25 years (mean [±SEM], 9.6 ±1.3). Age at the onset of asthma was from 0 to 33 years (mean, 10.5 ±1.8) and duration of symptomatic asthma was from 2 to 33 years (mean, 12.4±1.7). Remission of asthma had occurred in childhood in 12 subjects and followed cessation of a specific antigenic exposure to house pets in 9 subjects and after moving to another country in 2 others. Ten exasthmatics and two controls had past immunotherapy. Eleven asthmatics “in remission and 10 controls had a family history of asthma and, respectively, 16 and 21 subjects had a family history of atopy (Table 1).
Continue reading this post…
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission: Statistical Analysis
 Study Design
Study Design
The subjects came to the laboratory on three different occasions. On the first visit, one of the investigators administered a questionnaire on the characteristics of their former asthma (duration, severity, medication requirements, potential initiating factors, time of asthma diagnosis and of remission, including last 2 years’ respiratory symptoms, and family history of asthma). Lung volumes, expiratory flows, and bronchodilator response were measured. Skin prick tests with 26 common airborne allergens completed this first visit.
Measurements
The subjects were asked to measure their peak expiratory flow rates (PEFRs) with a peak flow meter (mini-Wright) twice daily for a 2-week period. They recorded on a diary card the results of three reproducible PEFR measurements in the morning and in the evening. Pulmonary function tests included three reproducible measurements of FEVi and forced vital capacity (FVC) before and after inhalation of albuterol (200 fig). Measurements were obtained with a spirometer (Vitalograph PTF II). Pulmonary volumes were measured by body plethysmography according to the method of Dubois et al. canadian neightbor pharmacy
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission: Methods
Subjects
Sixty-five subjects took part in this study (Table 1). Of these, 30 ex-asthmatics were recruited from advertisements in different media.
Inclusion Criteria and Definition of Asthma Remission
We included in the study men or women >18 years old, atopic or not, with a proven history of asthma responding to the American Thoracic Society criteria, who were considered to be in asthma remission for at least 2 years. “Remission” of asthma was defined according to the definitions of Bronnimann and Burrows: “asthma was considered to be inactive (ex-asthma) if the subject denied medications, asthmatic attacks, and ‘frequent’ (more than two) attacks of shortness of breath with wheezing during the preceding year.” We, however, extended the minimum period of symptom remission to 2 years, to be included in the study.
We considered that our subjects had “proven asthma” according to the following criteria: all had a history of dyspnea and wheezing in the past; 26 subjects had a diagnosis of asthma made by a physician; 16 had previous available chart recordings of typical asthma presentation and wheezing on chest auscultation; 27 had used antiasthma medications (mostly bronchodilators) for different periods of time; and physiologic data showing airflow obstruction were available in 10 subjects. Furthermore, ten subjects had been hospitalized previously for their asthma and five had required mechanical ventilation for acute asthma.
Continue reading this post…
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission
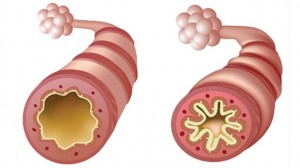 Bronchial asthma is characterized by variable airflow obstruction and airway hyperresponsiveness. Its underlying mechanism is considered to be an airway inflammatory process with bronchial epithelial damage and mucus secretion, and in which eosinophils and lymphocytes seem to play a key role.2 There is still no cure for asthma. We may, however, observe remissions, either spontaneously, after withdrawal of exposure to a sensitizing agent, or following bronchial anti-inflammatory therapy. Remissions are mostly observed in children, being quite rare in adults. Relapses of asthma after remission, however, are frequent in children. Blair reported a 20 percent recurrence of wheezing after a period of 3 years without symptoms in asthmatic children. Ryssing reported that in 36 percent of asthmatics who remitted from their asthma, wheezing resumed after a 13-year follow-up. In another study, 31 percent of young adults free of wheezing at 21 years old had recurrent wheezing at 28 years. mycanadianpharmacy.com
Bronchial asthma is characterized by variable airflow obstruction and airway hyperresponsiveness. Its underlying mechanism is considered to be an airway inflammatory process with bronchial epithelial damage and mucus secretion, and in which eosinophils and lymphocytes seem to play a key role.2 There is still no cure for asthma. We may, however, observe remissions, either spontaneously, after withdrawal of exposure to a sensitizing agent, or following bronchial anti-inflammatory therapy. Remissions are mostly observed in children, being quite rare in adults. Relapses of asthma after remission, however, are frequent in children. Blair reported a 20 percent recurrence of wheezing after a period of 3 years without symptoms in asthmatic children. Ryssing reported that in 36 percent of asthmatics who remitted from their asthma, wheezing resumed after a 13-year follow-up. In another study, 31 percent of young adults free of wheezing at 21 years old had recurrent wheezing at 28 years. mycanadianpharmacy.com
