Category
Competition for Intrathoracic Space Reduces Lung Capacity in Patients With Chronic Heart Failure: Discussion
These authors also suggest that, due to the increase in cardiac size, diffusion capacity of the lung suffers adversely, primarily as a consequence of a reduction in membrane diffusion as opposed to pulmonary capillary blood volume. Although moderate but significant correlations were observed between the cardiothoracic index and various components of pulmonary function, these findings may be underestimated for a number of reasons.
For instance, these authors only examined these relationships based on a one-dimensional measure of the thorax and heart. Also, they did not report data on the pulmonary thoracic index or other radio-graphically determined lung measurements. Thus, it is difficult to extrapolate these findings to true cardiac or lung volumes in relation to the volume of the thoracic cavity. The present investigation sought to expand this previous work and to gain a better understanding of the actual changes in cardiac volume in patients with stable chronic heart failure according to disease severity. In addition, we determined the impact that changes in cardiac volume have on lung volume using a three-dimensional volumetric analysis. Our results show a close association between the increase in cardiac volume and the loss of lung volume within a closed thoracic cavity, consistent with the restrictive pulmonary function pattern typically observed in heart failure patients. read
Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: Wasted Efforts
Racca et al recently studied the effectiveness of the helmet in a human model of resistive breathing, finding a higher inspiratory effort if the helmet was used compared to the face mask. In line with our data (Fig 5), the less effective unloading of the respiratory muscles in NIV-H was partially explained by the underassistance due to the long inspiratory delay time and the impaired pressurization rate during NIV-H. The pressurization may, however, be dependent on the amount of gas leakage and the maximal inspiratory flow of the respirator. Since gas leakage could almost completely be avoided in our lung model study, this may also offer an explanation for our favorable results regarding PTP with the use of a helmet.
In addition, rebreathing of CO2 with a helmet resulted in an almost doubled minute ventilation during resistive breathing and was therefore most likely the major cause for the increased work of breathing with the helmet. The problem of limited CO2 elimination has also been described in COPD patients, and was analyzed in an experiment showing increased CO2 concentrations within the helmet especially with demand flow systems. Both studies> imply that a continuous flow or flow-by system may be beneficial to reduce the inspiratory CO2 concentration and thus the risk of CO2 rebreathing. read only
Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: Inspiratory Effort
 With a helmet, the use of PS decreased delay times significantly, whereas this effect was relatively small during NIV-FM or invasive ventilation. These results suggest that the highest PEEP and PS levels clinically indicated and tolerated by the patient should be used when NIV with a helmet is used in order to enhance the trigger sensitivity. more
With a helmet, the use of PS decreased delay times significantly, whereas this effect was relatively small during NIV-FM or invasive ventilation. These results suggest that the highest PEEP and PS levels clinically indicated and tolerated by the patient should be used when NIV with a helmet is used in order to enhance the trigger sensitivity. more
The DelayPEEP seems to be important for patients with acute hypoxemic lung failure who continuously need a high alveolar distending pressure. Lungs collapse, and recruitment may occur rapidly on a breath-by-breath basis with time constants not longer than 400 ms. Depending on the PEEP and PS levels provided, DelayPEEP averaged between 81 ms and 397 ms. This time interval would allow collapse of unstable lung units with fast time constants. However, a decrease in Paw during a spontaneous inspiration is always secondary to an increase in the transpulmonary pressure, and should therefore not cause atelectasis.
Continue reading this post…
Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: Technical Aspects
The performance of our modern ICU ventilator was significantly affected by the use of a helmet designed for NIV because delay times were more than twice as long with a helmet compared to a face mask or invasive ventilation. The level of PS and CPAP had a major effect on delay times when a helmet was used, but not with a face mask or during invasive ventilation. In addition, PTP was smaller with NIV-H compared to NIV-FM or invasive ventilation, but not so when a complete inspiration with PS was evaluated. Wasted efforts occurred earlier during NIV-H and were aggravated with rising PS, RR, and compliance.
The data presented are based on trials in a mechanical lung model and are highly influenced by the compliance of the used interface and the degree of leakage. Repeated measurements with different helmets showed a relative wide range of measured time intervals due to varying compliance values of these helmets. Thus, delay times and PTPs reported in this study may vary if different helmets or tubing are used. The DelayTRlGGER was defined as the time interval between the initiation of an inspiration until the deflection of the Paw-time curve showed no further decrease in Paw, because the latter time point can easily and reliably be identified. other
Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: Delay Times
The second chamber, representing the “lung,” was connected to the tested ventilator (Evita 4; Drager Medical). The lung is passively displaced when the driving chamber is inflated by the ventilator. The following settings were studied: (1) RRs of10, 20, 30, and 40 breaths per minute; (2) PS levels raised in 1 cm H2O steps every minute until wasted inspiratory efforts occurred or up to a maximum of 30 cm H2O; (3) flow trigger set to 0.5 L/min and 15 L/min, respectively; and (4) respiratory compliance set at 30, 60, and 90 mL/cm H2O, respectively. The occurrence of wasted efforts was detected visually (failure of the ventilator-driven chamber to activate the passively driven lung chamber) and by analyzing the pressure volume curves off-line.
Statistical analysis was performed using self-programmed and commercially available software. Data are given as mean ± SD if not stated otherwise. Using a two-way analysis of variance, delay times and PTPs were analyzed for differences between the used interfaces (helmet vs mask vs endotracheal tube) and the applied PEEP or PS levels. If a significant difference was detected, a post hoc analysis using the Scheffe test was performed. A p level < 0.05 was considered to be significant. further
Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: Measurements of Time Delay
 To simulate spontaneous breathing, we used a modified lung model (LS1500; Drager Medical). This lung model consists of an electrically driven pneumatic lung simulator that allows the adjustment of tidal volume, RR, compliance, and resistance.
To simulate spontaneous breathing, we used a modified lung model (LS1500; Drager Medical). This lung model consists of an electrically driven pneumatic lung simulator that allows the adjustment of tidal volume, RR, compliance, and resistance.
To analyze the effect of the different interfaces on trigger sensitivity, effort, and the resulting PTPs, we defined three phases during the pressure curve (Fig 2): (1) the time interval (DelayTRlGGER), and the corresponding PTP interval between the initiation of an inspiration and the time point when the deflection of the Paw-time curve showed no further decrease in Paw (PTPtrigger); (2) the time interval from the initiation of an inspiration until the preset positive end-expiratory pressure (PEEP) was reached again (DelayPEEP), and the corresponding PTP from the initiation of an inspiration until the preset PEEP was reached again (PTPpeep); and (3) complete inspiration: during PS ventilation (PSV), the complete inspiration including the unassisted (DelayTRlGGER) and the pressurization segment was added to get the total PTP (PTP calculated over complete inspiration [PTPtot]). Flow and Paw were recorded with a sampling rate of 200 Hz. For the initiation of single breaths, data acquisition, and data analysis, specially programmed software was used. www.birthcontroltab.com
Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: Equipment
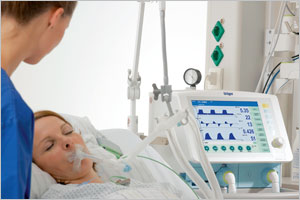
CPAP and NPSV were performed with a helmet (Starmed Castar R; Mirandola; Modena, Italy) or a face mask (King Systems Corporation; Noblesville, IN) put on a glass head that was connected to a lung model (Fig 1). The Castar R Helmet (size medium) has an internal volume of 7.5 L with inflated cuffs. When the head is inserted into the helmet, the internal volume is reduced to approximately 2.4 L due to the volume of the glass head used in this study. Two underarm laces attached to a ring at the lower site of the helmet should prevent the helmet from lifting when it is inflated. A plastic collar fitting around the neck prevents leakage during ventilation. Inspiratory and expiratory tube connectors are fitted in the upper part of the helmet.
The standard face mask (size medium, 125-mL internal gas volume) has an inflatable cushion fitted tightly to the head by dedicated rubber head straps. The cushion was inflated with 10 to 20 mL of air to adhere tightly to the glass head. When the mask is put on the head, the internal gas volume is reduced to approximately 100 mL.
Continue reading this post…
