Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Methods
Several technical abbreviations are used in the text (Table 1). Data were analyzed from diffusing capacity tests of patients referred to our outpatient pulmonary function testing laboratoiy. We did not screen the patients so that the patient population tested represents a typical sampling of patients referred to our laboratory for routine testing. The diffusing capacity was determined using an automated pulmonary function testing unit (Medical Graphics Corporation, St. Paul, Minn). When performing a test, the diffusion test gas mixture (0.3 percent CO, 0.5 percent Ne, 21 percent 02, and balance nitrogen) was first analyzed using a built-in gas chromatograph. Patients were instructed to exhale completely and then to rapidly inhale diffusion test gas and hold their breath for about 8 s. After breath hold, patients exhaled rapidly, during which the first 750 ml was discarded and the next 500 ml of expired gas was collected. In patients whose vital capacity was less than 2.0 L, the 500-ml sample was collected after 500 ml was expired. The expired gas sample was then drawn into the gas chromatograph for analysis of expired Ne and CO. Gas chromatography eliminates the need for a C02 correction.
Each maneuver was assessed for acceptability by the following requirements: inhaled volume < 90 percent of the largest vital capacity obtained in spirometry or lung volume determinations, total breath-hold time (Og) between 9 and 11s, time to inspire between 10 percent and 90 percent of the inhaled volume < 2.5 s, and time taken to collect the 500-ml “alveolar” gas sample < 3 s. A second maneuver was performed to check for reproducibility (Deo within 3 ml/min/mm Hg or 10 percent, whichever was larger) among acceptable maneuvers. If either reproducibility or acceptability of the first two maneuvers was not attained, a third was performed. In Tables 1 and 2, we report results from the average of acceptable maneuvers in the 283 patients satisfying all of the acceptability and reproducibility requirements. Data from the remaining 51 patients were used only for multiple regression analysis and are not included in average data. The methods we used differ in the presample washout volume and the collected volume of expired gas compared with the original descriptions of Ogilvie et al or Jones and Meade, though our methods for alveolar sample collection conform to the latest recommendations of the American Thoracic Society (ATS). Spirograms (Fig 1) were analyzed to obtain the times of the beginning of inspiration (the time of the first data point above minimum volume), the end of inspiration (the time of the first data point to attain maximum volume), the end of breath hold (the time of the first data point to decrease below maximum volume), and the beginning and end of sample collection. For multiple regression analysis, the total maneuver time (beginning of inspiration to the end of sample collection) was divided into IT (beginning of inspiration to end of inspiration), LT (end of inspiration to end of breath hold), and ET (end of breath hold to end of sample collection). Breath-hold times (BHT)- were determined by the methods of Og (beginning of inspiration to beginning of sample collection), JM (30 percent of inspiratory time to the middle of sample collection time) and ESP (50 percent of inspiratory volume to the beginning of sample collection).
Table 1—Abbreviations
| Abbreviation | Explanation |
| Pulmonary Function Variables | |
| TLC | Total lung capacity using body plethysmography |
| FVC | Forced vital capacity |
| FEV, | Forced expiratory volume in 1 s |
| Deo | Diffusing capacity (using Ogilvie timing method, unless otherwise stated) |
| Va | Alveolar volume (single-breath Ne dilution method) |
| IVC | Inspired vital capacity from Deo maneuver |
| Vos | Instrument (35 ml) plus assumed anatomic (150 ml) dead spaces |
| MI | Mixing index = (TLC – VJ/TLC |
| Deo timing methods (Fig 1) | |
| Og | Ogilvie |
| JM | Jones-Meade |
| ESP | Epidemiologic standardization project |
| 3PIT | 3-phase iterative, similar to 3-equation |
| Timing components (Fig 1) | |
| IT | Inspiratory time = end inspiration — begin inspiration |
| ET | Expiratory time = end sample collection — end breath hold |
| LT | Lockout time = end breath hold — end inspiration |
| BHT | Breath-hold times used in Deo calculations (equation 1, and lower panel, Fig 1) |
Table 2—Patterns of Pulmonary Function
| Pulmonary Function Category | TLC, % pred(9) | FVC, % pred (10) | FEV,, % pred (10) | FEV, /FVC, % | Deo, % pred(9) | MI,% |
| Normal n = 71 | 105 ±10 | 101 ±11 | 99±9 | 79 ±5 | 103 ±14 | 0.9±4.9 |
| Mild obstruction n = 52 | 107 ±12 | 89 ±9 | 71 ±6 | 63±5 | 89±23 | 9.6±8.2 |
| Moderate obstruction n = 36 | 109 ±15 | 75 ± 11 | 51 ±6 | 55±8 | 82 ±19 | 16.6 ±6.7 |
| Severe obstruction n = 25 | 123 ±20 | 58± 13 | 29±7 | 39 ±7 | 61 ±19 | 33.7 ±12.4 |
| Mild restriction n = 54 | 75 ±7 | 67 ±12 | 66± 14 | 79 ±8 | 69 ±23 | 4.7±8.3 |
| Moderate restriction n = 9 | 53±5 | 45±5 | 45±4 | 81 ±5 | 54± 18 | 4.8±5.7 |
| Reduced Deo n = 5 | 95± 10 | 96±9 | 94±4 | 82 ±6 | 77±4 | 4.4±5.2 |
| Reduced FVC, FEV, n = 31 | 97 ±9 | 84±7 | 79 ±5 | 77 ±6 | 90± 17 | 6.4±5.8 |
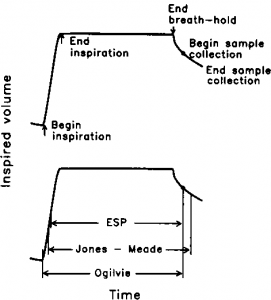
Figure 1. Definitions of timing components of the single-breath maneuver. Top panel shows a spirogram obtained from a maneuver to obtain a single-breath diffusing capacity of the lungs for carbon monoxide, with inhalation volume from bottom to top and time from left to right. This example from a patient with severe obstruction and prolonged expiratory time was chosen to illustrate timing components. Indicated times were used to calculate breath-hold times illustrated in the bottom panel. See Table 1 for definitions of ESP, Jones-Meade, and Ogilvie timings.