Influence of Two Different Interfaces for Noninvasive Ventilation Compared to Invasive Ventilation on the Mechanical Properties and Performance of a Respiratory System: PTPs
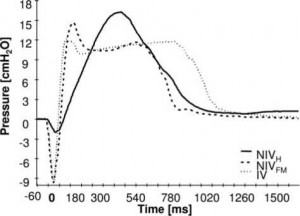
 During PS, the time course of Paw differed not only during the trigger phase but also later during pressurization (Fig 4). A rapid increase of Paw occurred after the trigger delay during NIV-FM and invasive ventilation, whereas this increase in Paw occurred more slowly during NIV-H. Consequently, PTP was slightly lower during the first 250 ms of inspiration with a helmet compared to NIV-FM and invasive ventilation, but not during the complete inspiration.
During PS, the time course of Paw differed not only during the trigger phase but also later during pressurization (Fig 4). A rapid increase of Paw occurred after the trigger delay during NIV-FM and invasive ventilation, whereas this increase in Paw occurred more slowly during NIV-H. Consequently, PTP was slightly lower during the first 250 ms of inspiration with a helmet compared to NIV-FM and invasive ventilation, but not during the complete inspiration.
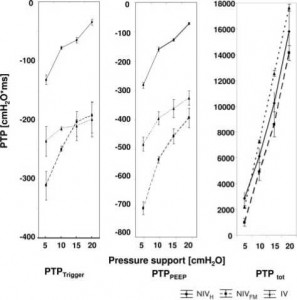
Interestingly, not only PTPtot but also PTPtrigger and PTPpeep were significantly influenced by the level of PS (p < 0.001) [Fig 5]. Mean PTPtrigger values averaged over all PS settings were significantly lower in NIV-H (mean, — 77 ± 41 cm H2O X s) than NIV-FM (mean, — 239 ± 54 cm H2O X s) or invasive ventilation (mean — 215 ± 15 cm H2O X s) [p < 0.001], and a similar pattern was observed for PTPpeep resulting in a significant difference for all PS settings in the post hoc analysis. However, there was no significant difference of average PTPtot values among NIV-H (mean, 8,744 ± 5,594 cm H2O X s), NIV-FM (mean, 7,161 ± 5,584 cm H2O X s) or invasive ventilation (mean, 9,902 ± 6,659 cm H2O X s), although significant differences between NIV-FM and invasive ventilation were observed at higher PS levels (Fig 5).
Influence of the Flow on Trigger Sensitivity
The influence of different flow triggers were tested with a PEEP of 8 cm H2O and a PS of 5 cm H2O and 15 cm H2O. Different flow triggers (0.5 L/min vs 5 L/min vs 15 L/min) had a significant influence on DelayTRlGGER, DelayPEEP, and the measured PTPs during NIV-H, while the effect on NIV-FM and invasive ventilation was minor. Reducing the flow trigger from 15 to 0.5 L/min caused a 20% reduction of DelayTRlGGER and a 14% reduction of DelayPEEP. PTPtrigger, and PTPpeep were decreased by 42% and 37%, respectively.
Wasted Efforts
The frequency of wasted inspiratory efforts increased with higher RRs, when the level of PS was increased, when the sensitivity of the flow trigger was decreased, and when the respiratory compliance increased (Table 1). In addition, the interface used for ventilation influenced the occurrence and frequency of wasted efforts, since wasted efforts were detected at lower PS levels and lower RRs in NIV-H compared to NIV-FM or invasive ventilation (Table 1).
Figure 4. Mean pressure course during PSV with NIV-H, NIV-fm, and endotracheal tube (invasive ventilation [IV]).
Figure 5. PTP before beginning of support of the ventilator (PTPtrigger), until set PEEP is reached (PTPpeep) and PTPtot over the whole unassisted and assisted phase at different PS levels.
Table 1—Influence of Lung Compliance and Flow Trigger on Occurrence of Wasted Efforts in NIV-fm and NIV-H Compared to Invasive Ventilation, at Different RRs
| Compliance, 30 mL/cm H2O | Compliance, 60 mL/cm H2O | Compliance, 90 mL/cm H2O | |||||||
| RR,breaths/min | NIV-H, cm H2O | NIV-fm | iInvasiveVentilation | INIV-H, cm H2O | NIV-fm, cm H2O | Invasive Ventilation, cm H2O | NIV-H, cm H2O | NIV-fm, cm H2O | Invasive Ventilation, cm H2O |
| Flow trigger at 0.5 L/min | |||||||||
| 10 | |||||||||
| 20 | 18 | 21 | 24 | ||||||
| 30 | 18 | 20 | 22 | 9 | 8 | 9 | |||
| 40 | 24 | 12 | 12 | 12 | 5 | 5 | 6 | ||
| Flow trigger at 15 L/min | |||||||||
| 10 | |||||||||
| 20 | 26 | 15 | 20 | 20 | |||||
| 30 | 28 | 14 | 17 | 20 | 6 | 7 | 7 | ||
| 40 | 18 | 8 | 10 | 11 | 4 | 5 | 5 | ||