Prospective Study of the Diagnostic Accuracy of the Simplify D-dimer Assay for Pulmonary Embolism in Emergency Department Patients: Discussion
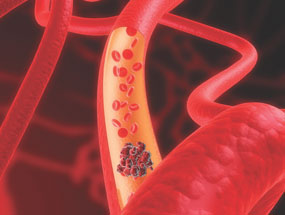 Figure 3 shows the plot of the likelihood ratio as a function of prevalence (R2 = 0.006 with t test on slope yielding p = 0.85; power to detect a significant correlation of 29%). The Pearson correlation coefficient observed for the plot of sensitivity vs prevalence yielded R2 = 0.20, with p = 0.27 from the t test on the slope; the plot of specificity vs prevalence yielded R2 = 0.38 with p = 0.10, and power of 36% (plots not shown). These regression analyses suggest the absence of a significant spectrum bias for either the pretest probability estimate or the underlying prevalence of PE on the diagnostic accuracy of the d-dimer assay. These computations do not address the possibility of spectrum effect, and the power to detect a significant relationship was small for each regression. This large, single-center study measured the diagnostic accuracy of a rapid, point-of-care, qualitative d-dimer assay in the ED setting. In a cohort of 2,302 patients, we found a moderate sensitivity of 80.5% and a relatively high specificity of 72.5%, leading to a negative likelihood ratio of 0.27. review
Figure 3 shows the plot of the likelihood ratio as a function of prevalence (R2 = 0.006 with t test on slope yielding p = 0.85; power to detect a significant correlation of 29%). The Pearson correlation coefficient observed for the plot of sensitivity vs prevalence yielded R2 = 0.20, with p = 0.27 from the t test on the slope; the plot of specificity vs prevalence yielded R2 = 0.38 with p = 0.10, and power of 36% (plots not shown). These regression analyses suggest the absence of a significant spectrum bias for either the pretest probability estimate or the underlying prevalence of PE on the diagnostic accuracy of the d-dimer assay. These computations do not address the possibility of spectrum effect, and the power to detect a significant relationship was small for each regression. This large, single-center study measured the diagnostic accuracy of a rapid, point-of-care, qualitative d-dimer assay in the ED setting. In a cohort of 2,302 patients, we found a moderate sensitivity of 80.5% and a relatively high specificity of 72.5%, leading to a negative likelihood ratio of 0.27. review
These findings are remarkably similar to the 81.8% sensitivity, 74.2% specificity, and negative likelihood ratio of 0.24 for the Simplify D-dimer assay recently reported by Hogg et al, who studied 417 adult ED patients in the United Kingdom who met an explicit definition of pleuritic chest pain. The criterion standard for the diagnosis of PE used by Hogg et al was very similar to ours. It therefore appears almost certain that the diagnostic accuracy of the Simplify D-dimer for PE differs significantly from the diagnostic accuracy of quantitative d-dimer assays used in ED populations with similar criterion standards. Systematic analyses have found the sensitivity and negative likelihood ratio of quantitative d-dimer tests at a cutoff of 500 ng/mL (either immunoturbidimetric or enzyme-linked immunoassay) to be approximately 93 to 94% and 0.12 to 0.15, respectively, when used to evaluate for PE in ED populations.- We examined the test characteristics of the Simplify D-dimer assay in an unselected, consecutive, nonconvenience sample of ED patients suspected of having PE. This fact and the lack of correlation between test performance vs stratification by pretest probability suggest that the relatively modest diagnostic performance of the Simplify D-dimer assay was probably not a result of spectrum bias.
We and others have stated the position that a safe d-dimer-based screening strategy to rule out PE in the ED should afford a posttest probability of PE < 1.0%. If the negative likelihood ratio of the Simplify D-dimer assay is very close to 0.27, then a negative d-dimer result could theoretically produce a posttest probability < 1.0% in any population with a pretest probability below (approximately) 3.5%.
Figure 3. Plot of the negative likelihood ratio as a function of prevalence of PE for eight different categories of pretest probability assessment.