Prospective Study of the Diagnostic Accuracy of the Simplify D-dimer Assay for Pulmonary Embolism in Emergency Department Patients: Results
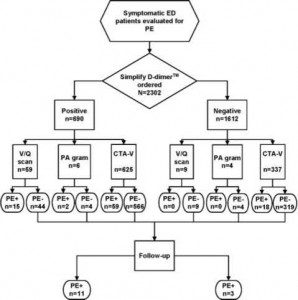
The d-dimer assay was performed on 2,302 patients enrolled from October 1, 2001, until June 30, 2004. Clinical characteristics of the study population are shown in Table 1. PE was diagnosed in 108 patients (4.7%; 95% CI, 3.6 to 5.6%). Figure 1 shows the flow diagram of diagnostic imaging relevant to PE. One thousand two hundred sixty-two patients with negative d-dimer results had no imaging performed, so the results of 90-day follow-up served as the criterion standard.
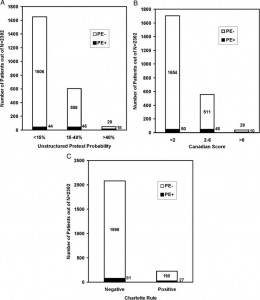
The distributions of pretest probability estimates from the unstructured approach, the Canadian score, and the Charlotte criteria are shown in Figure 2, which demonstrates that patients categorized as low risk for PE, either by the unstructured method < 15%, or by the Canadian score < 2, had a very low observed frequency of PE, at 2.7% (95% CI, 1.9 to 3.6%) and 2.9% (95% CI, 2.2 to 3.9%), respectively. When the Charlotte rule was negative, the frequency of PE was 3.9% (95% CI, 3.1 To 4.8%). read only
Table 2 shows the diagnostic 2 X 2 table results for the d-dimer assay in the entire cohort, for patients categorized as low risk by the unstructured method and the Canadian score, and for patients with a negative Charlotte rule. The sensitivity and specificity for the d-dimer assay in the entire cohort were 80.6% and 72.5%, respectively. These values did not change significantly when patients were selected on the basis of the three different pretest probability systems. If pretest probability was not considered, 1,612 patients in the entire cohort had negative d-dimer results, of whom 21 patients (1.3%; 95% CI, 0.8 to 2.0%) had PE. If we examine the effect of first stratifying for a low pretest probability, only one combination resulted in a posttest probability of PE < 1.0%: a low (< 15%) unstructured pretest probability estimate, plus a negative d-dimer result, which yielded a posttest probability of 0.7% (95% CI, 0.3 to 1.4%). To examine for possible spectrum bias, we plotted the sensitivity, specificity, and negative likelihood ratio as a function of the prevalence of PE that was observed in each of the eight different pretest probability strata: three each for the unstructured estimate and Canadian score, and two for the Charlotte rule. None of the regression plots demonstrated significant correlation.
Table 1—Clinical Characteristics of the Study Cohort (n = 2,302)
| Characteristics | Data |
| Vital signs | |
| Age, yr | 44.7 ± 15.8 |
| Respiratory rate, breaths/min | 21.1 ± 5.5 |
| Pulse rate, beats/min | 91.7 ± 19.6 |
| Systolic BP, mm Hg | 136.0 ± 25.1 |
| Room air arterial oxygen saturation, % | 97.3 ± 3.6 |
| Body temperature, °C | 36.7 ± 1.1 |
| Male gender | 703 (31) |
| Symptoms | |
| Pleuritic chest pain | 1,290 (56) |
| Dyspnea | 1,510 (66) |
| Substernal chest pain | 976 (42) |
| Syncope | 142 (6) |
| Cough | 749 (33) |
| Hemoptysis | 65 (3) |
| Risk factors and other conditions | |
| Surgery within prior 4 weeks | 105 (5) |
| Immobility! | 198 (9) |
| Prior DVT or PE | 171 (7) |
| Active malignancy | 179 (8) |
| Exogenous hormone use | 232 (10) |
| Pregnancy or postpartum within 4 wk | 100 (4) |
| History of coronary artery disease | 221 (10) |
| Congestive heart failure | 155 (7) |
| Asthma or COPD | 307 (13) |
| Current smoker | 862 (37) |
Table 2—Diagnostic Performance of the Simplify D-dimer Assay
| Assay Results | Criterion Standard Results! | |||
| IEntire Cohort (n = 2,302) | Unstructured Estimate < 15% (n = 1,650) | Canadian Score < 2 (n = 1,704) | Charlotte RuleNegative (n = 2,077) | |
| PE+ PE — | PE+ PE — | PE+ PE— | PE+ PE — | |
| Positive | 87 603 | 35 376 | 35 428 | 65 501 |
| Negative | 21 1,591 | 9 1,230 | 15 1,226 | 16 1,495 |
| Sensitivity | 80.6 (71.8-87.5) | 79.6 (64.7-90.2) | 70.0 (55.4-82.1) | 80.3 (69.9-88.2) |
| Specificity | 72.5 (70.6-74.4) | 76.6 (74.4-78.6) | 74.1 (71.9-76.2) | 74.9 (72.9-76.8) |
| Negative likelihood ratio | 0.27 (0.18-0.39) | 0.27 (0.15-0.45) | 0.40 (0.26-0.59) | 0.26 (0.17-0.40) |
| Negative predictive value | 98.7 (98.0-99.1) | 99.3 (98.6-99.6) | 98.8 (98.0-99.3) | 98.9 (98.3-99.4) |
| Negative posttest probability | 1.3 (0.8-2.0) | 0.7 (0.3-1.4) | 1.2 (0.7-2.0) | 1.1 (0.6-1.7) |
Figure 1. Flow diagram of diagnostic imaging performed in all patients. V/Q = ventilation/perfusion; PA gram = pulmonary angiogram; CTA-V = CT angiography-venography.
Figure 2. Distribution of pretest probability estimates derived the unstructured approach (top left, A), the Canadian Score (top right, B), and the Charlotte rule (bottom, C). The stacked bars show the total number of patients in each subcategory classified into patients without PE (open area) and patients with PE (filled area).