Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae: Research
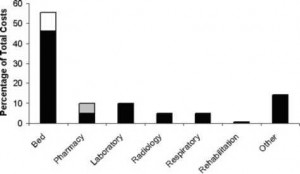
Only one patient received IV penicillin G, and the majority of (3-lactam use was cefuroxime, ceftriaxone, or cefepime. Eighty-three patients (49.4%) received an oral antibiotic during their hospital stay for the treatment of CAP, with all but two being transitioned from an IV regimen. A greater percentage of patients in the penicillin-susceptible group were transitioned from IV to oral compared with the nonsusceptible group, but the difference did not reach statistical significance (53.2% vs 38.6%, p = 0.137). For those patients who received oral therapy during hospitalization, the median day to transition was day 5 (25th to 75th percentile, day 4 to day 7). Penicillin susceptibility had no effect on the day to oral transition (p = 0.718). Total and departmental costs are depicted in Table 3. There was no significant difference on any cost level between patients infected with penicillin susceptible vs nonsusceptible S pneumoniae. The greatest percentage of total cost resources utilized were allocated to hospital bed costs (including both non-ICU and ICU beds) at 55.6%, followed by laboratory (9.9%) and pharmacy (9.8%) costs (Fig 1).
Antibiotics accounted for 48% of total pharmacy costs. Median costs were also not significantly different when separated into penicillin-susceptible, penicillin-intermediate, or penicillin-resistant S pneumoniae groups: $8,503 (25th to 75th percentile, $5,425 to $15,862) vs $6,347 (25th to 75th percentile, $4,889 to $13,099) vs $10,809 (25th to 75th percentile, $6,118 to $22,209), respectively (p = 0.477).
Independent variables included in the final multivariate models predicting total hospital costs and lengths of stay are shown in Table 4. Only baseline/ history of neoplasm, ICU admission, and delayed discharge were significantly associated with both higher total costs (adjusted r2 = 0.456) and increasing length of stay (adjusted r2 = 0.300). Additionally, hospital mortality (p = 0.039) was also associated with higher total costs, and baseline/history of CHF (p = 0.048) and presence of bacteremia (p = 0.026) also significantly predicted increasing length of stay. In both models, admission to the ICU had the greatest positive Р-coefficient, suggesting it was highly predictive of the dependent variables. Penicillin susceptibility was not significantly associated with total costs (p = 0.349) or length of stay (p = 0.409).
Table 3—Median Costs (2004 US$) by Cost Center for All Patients With CAP Caused by S pneumoniae and Then Comparable Results for Groups Defined by Penicillin Susceptibility
| Variables | All Patients(n = 168) | Patients With Penicillin-Susceptible S pneumoniae (n = 124) | Patients With Penicillin-Nonsusceptible S pneumoniae (n = 44) | p Valuef |
| Total costs | 8,654 (5,457-16,027) | 8,503 (5,425-15,862) | 9,441 (5,531-16,822) | 0.617 |
| Costs by cost center Non-ICU bed | 3,841 (2,379-6,124) | 3,827 (2,320-6,124) | 3,874 (2,764-5,835) | 0.740 |
| ICU bed | 0 (0-1,636) | 0(0-629) | 0 (0-3,282) | 0.460 |
| Pharmacy | 733 (462-1,379) | 744 (474-1,301) | 718 (459-1,695) | 0.853 |
| Antibiotics | 368 (259-642) | 365(256-606) | 372 (273-696) | 0.877 |
| Laboratory | 767 (498-1,588) | 821 (488-1,660) | 626 (507-1,482) | 0.537 |
| Radiology | 264 (115-999) | 256 (137-964) | 307 (86-1,605) | 0.986 |
| Respiratory care | 315(55-915) | 293 (72-826) | 336 (38-1,108) | 0.748 |
| Rehabilitation | 0(0-144) | 0(0-153) | 0 (0-167) | 0.817 |
| Other | 1,033 (601-2,682) | 1,029 (601-2,272) | 1,229 (662-3,096) | 0.350 |
Table 4—Final Multiple Linear Regression Models Predicting Total Hospital Costs and Length of Stay
| Independent Variables | Total Hospital Cost (Adjusted r2 = 0.46) | Length of Stay (Adjusted r2 = 0.30) | ||||
| Р Coefficient | SE | p Value | Р Coefficient | SE | p Value | |
| Age | – 0.001 | 0.002 | 0.502 | – 0.001 | 0.001 | 0.804 |
| Male gender | – 0.050 | 0.047 | 0.284 | – 0.076 | 0.04 | 0.079 |
| Diabetes | – 0.048 | 0.054 | 0.382 | – 0.035 | 0.050 | 0.486 |
| CHF | 0.124 | 0.066 | 0.061 | 0.121 | 0.061 | 0.048 |
| COPD | – 0.066 | 0.054 | 0.226 | – 0.061 | 0.050 | 0.223 |
| Neoplasm | 0.151 | 0.072 | 0.039 | 0.166 | 0.067 | 0.014 |
| Admission year | – 0.003 | 0.021 | 0.885 | 0.001 | 0.020 | 0.953 |
| Bacteremia | 0.082 | 0.048 | 0.091 | 0.100 | 0.044 | 0.026 |
| Delayed discharge | 0.172 | 0.052 | 0.001 | 0.165 | 0.048 | < 0.001 |
| ICU Admission | 0.512 | 0.055 | < 0.001 | 0.318 | 0.051 | < 0.001 |
| Mortality | 0.189 | 0.090 | 0.039 | 0.072 | 0.083 | 0.389 |
| Penicillin susceptibility | – 0.051 | 0.054 | 0.349 | – 0.041 | 0.050 | 0.409 |
| PSI score | 0.050 | 0.059 | 0.398 | 0.058 | 0.055 | 0.292 |
| Oral transition | 0.028 | 0.053 | 0.595 | 0.076 | 0.049 | 0.126 |
Figure 1. Percentage of total costs (2004 dollars) accounted for by each cost center. White area represents ICU bed costs, and gray area represents antibiotic costs.