The Third Epidemic—Multidrug-Resistant Tuberculosis: Results
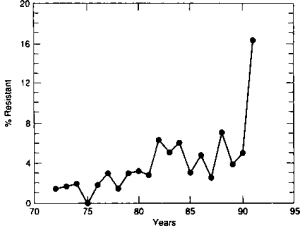
We analyzed the drug susceptibilities of 4,681 cases of ТВ from 1971 to 1991 at Bellevue Hospital Center, finding a dramatic increase in MDR-TB (isoniazid plus rifampin) in 1991 (Fig 1). There was an increase from a baseline of 2.5 to 16 percent combined isoniazid plus rifampin resistance in 1991. Among the 224 positive initial isolates collected over the first 6 months of 1991, the following drug resistances were found: 25 percent isoniazid, 20 percent rifampin, 17 percent streptomycin, and 14 percent ethambutol. Of these cases, 16 percent were isoniazid-plus-rifampin-resis-tant, and 13 percent were resistant to isoniazid, rifampin, streptomycin, and ethambutol. review
To define the clinical characteristics of this epidemic, we evaluated 100 consecutive DR-ТВ patients on the Chest Service and compared them to 54 randomly selected DS-TB patients over a 10-month period. Demographic data were similar in the DR-TB and DS-TB groups (Table 1). The patients we studied had a mean age of 40 years with 75 percent of the patients less than 44 years old. Ninety percent of the patients were male, and 85 percent were Hispanic or black. All of the patients admitted were unemployed, and approximately 65 percent were homeless.
Sixty-eight percent of patients admitted with DR-TB were IVDUs as compared with 55 percent with DS-TB. Fifty-five percent of the patients admitted with DR-TB were HIV-positive versus 53 percent with DS-TB (Table 1). Forty percent of the patients had a previous history of active ТВ diagnosed at another New York City Hospital in the previous 2 years. Of the cases that were isoniazid-plus-rifampin-resistant, 50 percent had previous anti-ТВ treatment. However, there appeared to be increased susceptibility in immunocompromised persons to DR-TB in that 77 percent of those patients who were HIV-positive and had DR-TB had no previous treatment.
Clinically, few differences were evident between those patients with DR-TB versus those with DS-TB (Table 2). Thirty-three percent with DR-TB exhibited anergy versus only 8 percent of those with DS-TB (p<0.05). Forty-five percent of DR-TB patients exhibited fever versus 30 percent of DS-TB patients. Cough was present in 40 percent of DR-TB versus 30 percent of DS-TB patients. With regard to night sweats, 24 percent of those who had DR-TB experienced them, versus 14 percent with DS-TB. Weight loss was reported by 30 percent of those with DR-TB and 26 percent of those with DS-TB. The chest radiograph commonly revealed bilateral infiltrates, adenopathy, and cavities, with similar percentages in both groups (Table 2). Opportunistic infections were surprisingly infrequent: there were 16 documented episodes of Pneumocystis carinii pneumonia, 3 of toxoplasmosis, 5 of cryptococcosis, 4 of M avium, and 4 of extrapulmonary tuberculosis spread equally among the 2 study groups.
Figure 1. Combined isoniazid and rifampin resistance.
Table 1—Demographic Characteristics of Drug-Resistant vs Drug-Sensitive Tuberculosis Fatients at Bellevue
| Characteristic | Drug-Resistant,% | Drug-Sensitive,% |
| Age, yr (mean) | 40 | 39 |
| Black or Hispanic | 85 | 80 |
| Male | 90 | 90 |
| Intravenous drug abuser | 68 | 55 |
| Homeless | 65 | 68 |
| HIV-positive | 55 | 53 |
| Unemployed | 100 | 100 |
| Previous ТВ | 40 | 40 |
Table 2—Clinical Characteristics of Drug-Resistant vs Drug-Sensitive Tuberculosis Fatients at Bellevue
| Clinical Parameter | Drug-Resistant,% | Drug-Sensitive,% | PValue* |
| Anergy | 33 | 8 | <0.05 |
| Fever | 45 | 30 | NS |
| Cough | 40 | 30 | NS |
| Night sweats | 24 | 14 | NS |
| Wfeight loss | 30 | 26 | NS |
| Chest radiograph: | |||
| Bilateral infiltrate | 55 | 45 | NS |
| Adenopathy | 20 | 15 | NS |
| Cavities | 30 | 32 | NS |
| Miliary | 5 | 1 | NS |
| Normal | 6 | 6 | NS |