Category - Part 18
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Discussion
 Our study shows the following results:
Our study shows the following results:
(1) In patients with DMD, respiratory muscles and in particular the diaphragm, are trainable in terms of strength and endurance, provided that their ventilatory function is not severely restricted.
(2) In patients with VC values less than 25 percent predicted and/or a PaC02 of more than 45 mm Hg, a specific training of the inspiratory muscles does not produce any benefit. On the other hand, a damaging effect could be excluded, at least for a training period of 1 month.
The significance of skeletal muscle training in patients with neuromuscular disease is controversial. There is a scarcity of data regarding whether or not diseased muscles can be strengthened by specific training programs at all, much less the exact extent and stage of the disease at which skeletal muscles can be strengthened. In one patient with Duchenne dystrophy, histologic examination showed that those muscles assuming the least degree of sustained physical activity had the least degeneration, implying that physical activity hastened muscle fiber degeneration. It was therefore suspectpd that overwork or heavy exercise may accelerate skeletal muscle weakness in neuromuscular disease. my canadian pharmacy phone number
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Analisys
At the beginning of the study the Pesmax and Pdimax values were not significantly different in the two groups (Fig 1, Table 2). After the 6-month training period, however, the ten patients who completed the training had significantly higher Pesmax and Pdimax values than the 12 control subjects without severe functional impairment (p < 0.001) (Fig 1, Table 2). At the end of training the mean Pesmax and Pdimax values were 5.59 ± 0.98 kPa and 6.61 ±1.16 kPa, respectively, for the 10 training patients; 3.38 ± 1.18 kPa and 4.12 ± 1.11 kPa, respectively, for the 12 controls. The 12 controls without severe pulmonary function impairment, the 5 training, and the 3 control patients with severe impairment showed no significant change of Pesmax and Pdimax values during the observation period (Fig 1, Table 2). The effects of training on inspiratory muscle endurance are shown in Table 3. In the ten patients who completed the training, the endurance time increased significantly (Table 3). The reasons for terminating the test are also listed in Table 3. It should be noted that in the ten patients who completed the training, the target pressure during the resistive breathing tests increased during the training period. This means that the inspiratory task which could be sustained increased. In these ten patients, a pressure/endurance-time product was calculated by multiplying the created Pdi by Те to compare the work capacity of the inspiratory muscles before and at the end of training. The mean pressure-time product increased from 2678 kPa«s to 5500 kPa«s (p < 0.001) (Fig 2). sildenafil citrate pink
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Results
 The mean of the five highest pressure values during ten maximal static inspiratory efforts against the almost occluded airway was used as the minimal pressure value which had to be reached during such efforts at home. This value had to be adjusted each month anew, if the patients could meanwhile achieve higher mean pressure values. If a training patient showed no improvement in the inspiratory muscle function parameters after 1 month of training, he met our discontinuation criterion and was excluded from the study, since significant improvement should have occurred within 1 month. Data Analysis
The mean of the five highest pressure values during ten maximal static inspiratory efforts against the almost occluded airway was used as the minimal pressure value which had to be reached during such efforts at home. This value had to be adjusted each month anew, if the patients could meanwhile achieve higher mean pressure values. If a training patient showed no improvement in the inspiratory muscle function parameters after 1 month of training, he met our discontinuation criterion and was excluded from the study, since significant improvement should have occurred within 1 month. Data Analysis
The baseline parameters of the two groups were compared by means of the Mann-Whitney test. The changes during the training period within one group were compared by the Wilcoxon test. The Spearman rank correlation coefficient was used to test the relationship between improvement in respiratory muscle strength and endurance and baseline levels of VC. canadian neightbor pharmacy
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Protocol
The catheters were perfused with distilled water at a constant flow of 25 ml/h. The proximal ends were coupled to pressure transducers (Could-Statham, P23ID, Cleveland). The catheter-pressure transducer system was described in detail previously. The Pdi was calculated by subtracting esophageal pressure (Pes) from the gastric pressure (Pga) by an electronic subtraction circuit. The Pes, Pga, and Pdi were displayed on-line on a four-channel paper recorder (Beckman 511 A, Fullerton, Calif). The Pes, Pga, and Pdi were arbitrarily assigned zero at the start of each sniff trial. Thus, only the change in pressure from the initial position was determined for each sniff. An interval of 30 to 40 s was allowed between e ach sniff and the best of a total of ten maneuvers was used for analysis. buy allegra
Inspiratory Muscle Endurance: The patients were instructed to breathe continuously in cycles at a certain level of inspiratory resistance for 1 min, followed by 20 s of rest. The test was terminated when the Pdi could not be sustained at the target level for three consecutive breaths or when a total of 20 resistive breathing cycles were completed by the patient. The cumulative time of these maneuvers (Те) served as a parameter for inspiratory muscle endurance. A single-lead ECG was monitored throughout the maneuvers. The blood gas values assessed immediately after the resistive breathing cycles showed no worsening in oxygen tension or increase in C02 tension in any patient.
Continue reading this post…
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Inspiratory Muscle Training at Home
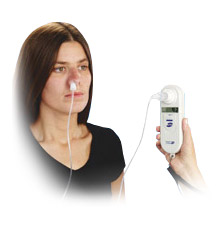 At home, patients had to perform both resistive breathing maneuvers and maximal static inspiratory efforts against the almost occluded resistance. Training was done in the sitting position and a noseclip was used. The inspiratory resistive breathing training consisted of ten loaded breathing cycles of 1-min duration each, with 20-s intervals between them, twice daily. The level of the inspiratory resistance was adjusted in the hospital. During the 1-min resistive breathing cycle, if the minimal airflow value was not achieved more than two times, a warning signal on the training apparatus would be shown to the patient and the cycle had to be repeated. The same happened if the desired Ve was not achieved. Thus, each patient had to correctly complete ten resistive breathing cycles twice a day. The number of correctly and incorrectly performed exercises was stored in the apparatus. Fifteen minutes after the resistive breathing training, the patients had to perform ten maximal static inspiratory efforts and reach a certain minimal pressure value, which was determined in the hospital. A 20-s interval between the maneuvers was allowed. When the minimal pressure value was not achieved, this maneuver had to be repeated, until a total of ten maneuvers were performed correctly. The number of correctly and incorrectly performed efforts was stored in the apparatus. canada health and care mall
At home, patients had to perform both resistive breathing maneuvers and maximal static inspiratory efforts against the almost occluded resistance. Training was done in the sitting position and a noseclip was used. The inspiratory resistive breathing training consisted of ten loaded breathing cycles of 1-min duration each, with 20-s intervals between them, twice daily. The level of the inspiratory resistance was adjusted in the hospital. During the 1-min resistive breathing cycle, if the minimal airflow value was not achieved more than two times, a warning signal on the training apparatus would be shown to the patient and the cycle had to be repeated. The same happened if the desired Ve was not achieved. Thus, each patient had to correctly complete ten resistive breathing cycles twice a day. The number of correctly and incorrectly performed exercises was stored in the apparatus. Fifteen minutes after the resistive breathing training, the patients had to perform ten maximal static inspiratory efforts and reach a certain minimal pressure value, which was determined in the hospital. A 20-s interval between the maneuvers was allowed. When the minimal pressure value was not achieved, this maneuver had to be repeated, until a total of ten maneuvers were performed correctly. The number of correctly and incorrectly performed efforts was stored in the apparatus. canada health and care mall
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Training Apparatus
For this study, a special training apparatus was constructed to enable the patient to actually adhere to the prescribed training intensity. In addition, the number of correctly and incorrectly performed exercises was stored by the apparatus to give the physician the possibility to control the training of the patient.
The training apparatus enabled the patient to do resistive breathing maneuvers against a variable inspiratory resistance or maximal static inspiratory efforts against the almost occluded resistance. Room air was breathed through a mouthpiece, a twoway non-rebreathing valve of low resistance, a 3-cm-long plastic tube, a pneumotachograph, and a variable alinear inspiratory resistance. Inspiratory flow was measured with the pneumotachograph connected to a differential pressure transducer (Honeywell 163 PC, Freeport, III). The training equipment was kept in a small collapsible case. In the bottom half of the case, the mouthpiece, the two-way valve, and the short plastic tube were kept. The pneumotachograph and the alinear resistor were fixed in this part of the case. In addition, there was a slot for a videogame cassette that could be opened if the training was successful. The possibility to play a videogame as a reward could motivate the patients not to interrupt the training prematurely. mycanadianpharmacy
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Methods
 One of the main problems in the treatment of patients with neuromuscular diseases is the progressive impairment of inspiratory muscle function. Since chest wall and pulmonary compliance are reduced in neuromuscular diseases, the mechanical load on the weakened respiratory muscles is increased. Imbalance between load and capacity of the respiratory muscles may lead to fatigue and respiratory failure, which is the most important cause of death in these patients. Therefore, the treatment of diseased respiratory muscles to improve their strength and endurance presents a great challenge in the treatment of patients with neuromuscular diseases. Pharmacologic therapy was reported to possibly strengthen the respiratory muscles and make them less susceptible to fatigue. Also, periodic respiratory muscle rest and training were used to prevent the decline in respiratory muscle function. canadianfamilypharmacy
One of the main problems in the treatment of patients with neuromuscular diseases is the progressive impairment of inspiratory muscle function. Since chest wall and pulmonary compliance are reduced in neuromuscular diseases, the mechanical load on the weakened respiratory muscles is increased. Imbalance between load and capacity of the respiratory muscles may lead to fatigue and respiratory failure, which is the most important cause of death in these patients. Therefore, the treatment of diseased respiratory muscles to improve their strength and endurance presents a great challenge in the treatment of patients with neuromuscular diseases. Pharmacologic therapy was reported to possibly strengthen the respiratory muscles and make them less susceptible to fatigue. Also, periodic respiratory muscle rest and training were used to prevent the decline in respiratory muscle function. canadianfamilypharmacy
Previous studies have shown that strength and endurance of the respiratory muscles can be improved through specific training programs in normal subjects, patients with COPD, patients with cystic fibrosis, and quadriplegics. However, the role of inspiratory muscle training remains controversial in patients with neuromuscular diseases. On the one hand, it is alleged that inspiratory muscle training is potentially hazardous, since it may accelerate fatigue in the already very weak respiratory muscles by overwork and therefore cannot be recommended. On the other hand, improvement of inspiratory muscle function by specific training programs has been reported, but these studies were uncontrolled. The question of whether the use of inspiratory muscle training is sensible remains unanswered. And if the answer is yes, when should we intervene in the course of the patient’s disease?
The goal of our study is to answer the following questions: (1) Does respiratory muscle training in patients with Duchenne muscular dystrophy (DMD) improve inspiratory muscle function or does it do more harm? (2) Does the severity of the existing pulmonary function impairment affect the obtainable training effects?
Continue reading this post…
