Category - Part 19
Mucosa-Associated Lymphoid Tissue Lymphoma of the Lung With Cold-reacting Autoantibody-mediated Hemolytic Anemia – Discussion
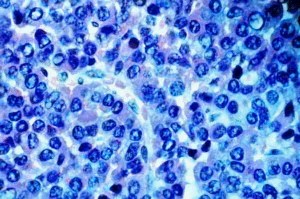
The concept of MALToma was first described bv Isaacson and Wright2 in a patient suffering from immunoproliferative intestinal disease and low-grade primary В cell lymphoma of the stomach in 1983. The distinct clinicopathologic entity was later extended to include low-grade В cell lymphoma arising from other mucosal organs including the bronchus, salivary gland, thyroid gland, thymus, orbital organs, bladder, and female genital tract. Pulmonary MALToma is very rare and often difficult to diagnose. It may have a mixed population of small lymphocytes and plasma cell infiltration at the submucosal area, even associated with germinal center formation. Usually it is misdiagnosed as a pseudolymphoma. However, demonstration of typical angulated centrocyte-like lymphoid cells and lymphoepithelial lesions would be characteristic for histologic diagnosis of a MALToma. The dominant component is a diffuse infiltrate of small-to-intermediate-sized В lymphoid cells with irregular nuclei and pale to clear cvtoplasma, which are called “centrocytelike cells” or “monocytoid В cells.” Lymphoid follicles are scattered throughout the infiltrate, which may be distorted or even overrun by the surrounding centrocyte-like cells. Immunohistochemical staining establishes the presence of \ or к light chain restriction within the infiltrate of mono-typic В cells.
Continue reading this post…
Mucosa-Associated Lymphoid Tissue Lymphoma of the Lung With Cold-reacting Autoantibody-mediated Hemolytic Anemia – Case Report
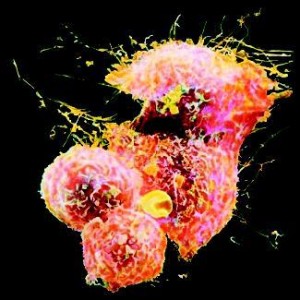 The primary mucosa-associated lymphoid tissue lymphoma (MALToma) of the lung is a rare low-grade В cell lymphoma arising from bronchus-associated lymphoid tissue which had been regarded as pseudolymphoma. It has characteristic histologic findings with monoclonal В cells of centrocytelike lymphoid cells and a lymphoepithelial lesion. This is a case report of MALToma of the lung and cold-reacting autoantibody-mediated hemolytic anemia. To our knowledge, there is no other report of such an association in the English-language medical literature. A morphologic and immunohistologic analysis of the case demonstrates the variety of distinctive histologic features ascribed to low-grade lymphoma of pulmonary MALT, which is consistent with the histologic details of MALToma arising from a variety of other glandular epithelial tissues.
The primary mucosa-associated lymphoid tissue lymphoma (MALToma) of the lung is a rare low-grade В cell lymphoma arising from bronchus-associated lymphoid tissue which had been regarded as pseudolymphoma. It has characteristic histologic findings with monoclonal В cells of centrocytelike lymphoid cells and a lymphoepithelial lesion. This is a case report of MALToma of the lung and cold-reacting autoantibody-mediated hemolytic anemia. To our knowledge, there is no other report of such an association in the English-language medical literature. A morphologic and immunohistologic analysis of the case demonstrates the variety of distinctive histologic features ascribed to low-grade lymphoma of pulmonary MALT, which is consistent with the histologic details of MALToma arising from a variety of other glandular epithelial tissues.
A 39-year-old Chinese woman was admitted to National Taiwan University Hospital in May 1992 with a 2-year history of chronic productive cough accompanied by yellowish sputum. The chest radiograph showed diffuse alveolar consolidations in both lungs (Fig 1). The patient had received antituberculosis therapy for 1 year without improvement in 1991. She had been hospitalized elsewhere without a definite diagnosis, even by transbronchial lung biopsy, 1 year prior to admission. Dyspnea and intermittent fever gradually developed in addition to the productive cough.
Continue reading this post…
Comparison of Cardiac Pacing Modes in Patients With Chronic Obstructive Pulmonary Disease – Discussion
Dyspnea with exertion is a commonly recognized complaint in patients with lung disease. An increasing perception of shortness of breath with exercise is consistent with severe lung disease and frequently results in a fear of exertion that not only limits any activity requiring exertion, but daily living activities as well. The limitation of physical activities also leads to deconditioning, which then further compromises the patient’s ability to exercise. It has been shown that individual perceptions of dyspnea are very subjective and correlate better with work of breathing rather than level of hypoxemia. Due to the relative subjectivity of the complaint, “I feel short of breath with exercise” and the fact that most patients will modify their life-styles to accommodate increasing dyspnea with exertion, providing medical management that will keep these patients active and clinic ally stable is a challenge. Any adjunct that can help to optimize oxygen delivery is valuable in the treatment and rehabilitation of these patients. buy birth control
In this study, those patients with chronic lung disease who required cardiac pacing performed significantly better with a DDRR as compared with WIR. There was a significant improvement in exercise duration as well as a decrease in the ventilatory equivalents for oxygen at all levels of exercise. The improvement in exercise duration is important as it suggests an increased exercise tolerance. One must also be careful not to overlook the significance of the decreases seen in the ventilatory equivalent for oxygen at all levels of exercise. This decrease is consistent with a trend toward improvement in AT, suggesting a decrease in lactic acid production throughout exercise and an improvement in the efficiency of oxygen delivery with this mode. Perhaps even more important is that decreases in ventilator)’ effort or work of breathing will affect the patient’s perception of dyspnea. All of the patients with COPD we tested stated that they felt less short of breath during exercise with the DDDR pacing mode compared with the WIR mode, which is consistent with the decreases noted in ventilatory equivalents for oxygen at all levels of exercise.
Continue reading this post…
Comparison of Cardiac Pacing Modes in Patients With Chronic Obstructive Pulmonary Disease – Results
 All patients with COPD had sinus node dysfunction, including four with chronotropic incompetence. All had AV nodal disease, three 3° AV block, four 1° AV block, and one 2° AV block. Three of these patients had documented retrograde conduction and a history of pacemaker syndrome in the WI mode. However, only one of these patients demonstrated a symptomatic pacemaker syndrome, that is, retrograde conduction and a drop in blood pressure during testing in this study. In patients with normal lung function, all had sinus node disease, including seven with chronotropic incompetence, four had AV nodal disease, one had 3° AV block, and three had 1° AV block. Two patients had demonstrated retrograde conduction in the WWVIR mode during testing in this study, though they did not have a simultaneous fall in blood pressure. Both of these patients had a documented history of pacemaker syndrome in the WI mode. An additional three patients in this group had a documented history of pacemaker syndrome in the WI mode, but this was not observed during testing in this study (Table 1). No cardiac arrhythmias occurred during exercise, and there were no adverse pacemaker interactions with underlying rhythms. asthma inhalers
All patients with COPD had sinus node dysfunction, including four with chronotropic incompetence. All had AV nodal disease, three 3° AV block, four 1° AV block, and one 2° AV block. Three of these patients had documented retrograde conduction and a history of pacemaker syndrome in the WI mode. However, only one of these patients demonstrated a symptomatic pacemaker syndrome, that is, retrograde conduction and a drop in blood pressure during testing in this study. In patients with normal lung function, all had sinus node disease, including seven with chronotropic incompetence, four had AV nodal disease, one had 3° AV block, and three had 1° AV block. Two patients had demonstrated retrograde conduction in the WWVIR mode during testing in this study, though they did not have a simultaneous fall in blood pressure. Both of these patients had a documented history of pacemaker syndrome in the WI mode. An additional three patients in this group had a documented history of pacemaker syndrome in the WI mode, but this was not observed during testing in this study (Table 1). No cardiac arrhythmias occurred during exercise, and there were no adverse pacemaker interactions with underlying rhythms. asthma inhalers
Comparison of Cardiac Pacing Modes in Patients With Chronic Obstructive Pulmonary Disease – Methods
Spirometry was used to evaluate baseline lung function for each patient. This was performed prior to exercise, with the patient standing. Patients were required to perform three reproducible forced expiratory and inspiratory maneuvers. All patients were then evaluated with paired exercise testing using the Chronotropic Assessment Exercise Protocol Pulmonary gas exchange, exercise duration, heart rate, and rhythm were measured during exercise.
Although there may be some variability in exercise results with serial testing when several exercise tests are done on the same day or on different days, attempts were made to minimize any inadvertent bias by random selection of the pacing modes and strict adherence to the study protocol. A minimum of 2 h was allowed between each exercise study. Cardiac output was obtained at rest and immediately after maximum exercise using echo-Doppler techniques. Stroke volume was determined from the flow velocity integral recorded with the Doppler sample volume positioned in the left ventricular outflow tract. Cardiac output determination by echo-Doppler technique has been shown to be reliable in measuring qualitative changes. buy claritin online
Comparison of Cardiac Pacing Modes in Patients With Chronic Obstructive Pulmonary Disease – Patient Population
 Limitations in exercise tolerance are a common manifestation of patients with chronic lung disease. Compromised pulmonary mechanics limit the ability of the lungs to respond to increasing oxygen demands. This leaves these patients dependent on other mechanisms to deliver available oxygen to the tissues to support the metabolic demands of exercise. Optimizing cardiac output is, therefore, important to provide maximum oxygen delivery. This is no less important for patients with moderate to severe lung disease who develop symptomatic bradycardia and require implantation of a cardiac pacemaker. This study was designed to compare the relative efficacy in optimizing cardiac performance and exercise capacity of two different cardiac pacing modes. The relatively complex dual chamber adaptive rate pacing (DDDR) was compared with the significantly simpler ventricular adaptive-rate pacing (WIR) in patients with lung disease who require pacemaker implantation for symptomatic bradycardia. buy flovent inhaler
Limitations in exercise tolerance are a common manifestation of patients with chronic lung disease. Compromised pulmonary mechanics limit the ability of the lungs to respond to increasing oxygen demands. This leaves these patients dependent on other mechanisms to deliver available oxygen to the tissues to support the metabolic demands of exercise. Optimizing cardiac output is, therefore, important to provide maximum oxygen delivery. This is no less important for patients with moderate to severe lung disease who develop symptomatic bradycardia and require implantation of a cardiac pacemaker. This study was designed to compare the relative efficacy in optimizing cardiac performance and exercise capacity of two different cardiac pacing modes. The relatively complex dual chamber adaptive rate pacing (DDDR) was compared with the significantly simpler ventricular adaptive-rate pacing (WIR) in patients with lung disease who require pacemaker implantation for symptomatic bradycardia. buy flovent inhaler
The Third Epidemic—Multidrug-Resistant Tuberculosis: Discussion
 During the past decade, the incidences of HIV infection and ТВ have ascended to epidemic proportions in several major US cities. At Bellevue Hospital Center in Manhattan, the incidence of MDR-TB has increased sevenfold in 1991 as compared with any of the previous 20 years. buy antibiotics online
During the past decade, the incidences of HIV infection and ТВ have ascended to epidemic proportions in several major US cities. At Bellevue Hospital Center in Manhattan, the incidence of MDR-TB has increased sevenfold in 1991 as compared with any of the previous 20 years. buy antibiotics online
Several case series have been reported by the Centers for Disease Control in which M tuberculosis isolates were resistant to first-line anti-ТВ medications. In a cooperative Centers for Disease Control-New York City Department of Health study, 466 cultures positive for M tuberculosis were tested for drug susceptibilities from laboratories throughout the city collected during April 1991. Thirty-three percent had resistance to one or more anti-ТВ drugs and almost 20 percent had resistance to both isoniazid plus rifampin. Patients who were currently or previously treated with anti-ТВ drugs were more likely to have resistant organisms than those who had not been previously treated. Of isolates obtained from Bellevue for this cooperative study, 13 of 50 (26 percent) were resistant to both isoniazid plus rifampin, suggesting that our reported rates may actually be underestimates. Chawla and colleagues found an overall resistance rate of 30.9 percent to one or more drugs at Kings County Hospital in Brooklyn. More than half (56.6 percent) of those resistant were resistant to more than one drug. They found a combined pattern of isoniazid-plus-rifampin resistance in 30.2 percent of cases. Our results showed an overall resistance rate of 33 percent, and also that patients were most commonly resistant to isoniazid (25 percent) followed by rifampin (20 percent). Our patient population showed a similar distribution with an isoniazid-rifampin resistance of 16 percent and an isoniazid-rifampin-streptomycin-ethambutol resistance of 13 percent. These figures are especially disturbing, since the case fatality rate for MDR-TB exceeds 50 percent, and approaches 90 percent among HIV-positive individuals.
Continue reading this post…
