Category - Part 17
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Discussion
Our main findings are as follows: (1) the singlebreath Deo was largest using the ESP timing method compared with JM, 3PIT, and Og methods (in decreasing order of mean Deo); (2) the difference between Deo using Og, JM, and 3PIT methods was small in patients with normal pulmonary function and became less in patients with obstruction, restriction, or low Deo; and (3) the reproducibility of Deo for replicate maneuvers was equivalent among the four methods. The differences among JM, Og and ESP timings reside in differences in definition of start and end of breath hold (Fig 1). Using backward elimination of nonsignificant terms, only IT and ET remained a significant term in the multiple regression models comparing Deo by Og, ESP, and JM (Table 4). The ESP gives the largest Deo in all patient groups because it uses the shortest breath hold time, start of breath hold being generally later than Og and JM, and end of breath hold at beginning of sampling. The Og is smallest in patients with normal expiratory flows because the Og inspiratory time is always larger than the others, due to the earlier start of breath hold. In normal individuals the differences between JM and both Og and ESP definitions for end of breath hold were insignificant. canadianneighborpharmacy.com
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Results
 The mean percents of predicted values for pulmonary function variables are listed in Table 2, categorized by pulmonary function abnormalities. Mean and SD values for Deo and the mean WP-SD of Deo by the various protocols are listed in Table 3 using the same categorization. The ESP protocol resulted in the largest Deo, followed by the JM and 3PIT methods, with Og resulting in the smallest Deo in most categories. The differences among Deo by various timing methods was significant (p < 0.01) for all paired comparisons in the group with normal patterns of pulmonary function. In other categories, the differences were generally less, and statistical significance was not attained in a number of comparisons. The JM and 3PIT Dcos were not significantly different in moderate to severe obstruction, restriction, or reduced Deo patient groups. The JM was less than ESP Deo in all patient groups except moderate restriction and isolated reduced Deo. The Og remained significantly less than JM, ESP, and 3PIT Dcos in all groups except in the moderate restriction and reduced Deo groups, where Og and 3PIT Dcos were not significantly different. The intrasubject SD of Deo was generally not significantly different among groups (p > 0.01) with the exception of the 3PIT method that gave the least reproducible Deo in the group with mild restriction. buy tavist online
The mean percents of predicted values for pulmonary function variables are listed in Table 2, categorized by pulmonary function abnormalities. Mean and SD values for Deo and the mean WP-SD of Deo by the various protocols are listed in Table 3 using the same categorization. The ESP protocol resulted in the largest Deo, followed by the JM and 3PIT methods, with Og resulting in the smallest Deo in most categories. The differences among Deo by various timing methods was significant (p < 0.01) for all paired comparisons in the group with normal patterns of pulmonary function. In other categories, the differences were generally less, and statistical significance was not attained in a number of comparisons. The JM and 3PIT Dcos were not significantly different in moderate to severe obstruction, restriction, or reduced Deo patient groups. The JM was less than ESP Deo in all patient groups except moderate restriction and isolated reduced Deo. The Og remained significantly less than JM, ESP, and 3PIT Dcos in all groups except in the moderate restriction and reduced Deo groups, where Og and 3PIT Dcos were not significantly different. The intrasubject SD of Deo was generally not significantly different among groups (p > 0.01) with the exception of the 3PIT method that gave the least reproducible Deo in the group with mild restriction. buy tavist online
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Standard Deviation
Predicted values were taken from Miller et al for Deo and TLC, and Miller for FVC and FEV,. Standing height (cm) without shoes and weight (kg) were measured immediately prior to pulmonary function evaluation. These categories are used as a framework within which to illustrate the dependence of the differences among Deo values on pulmonary function abnormality. The “normal” category is narrowly defined, with a higher cutoff than the example given by the ATS and probably higher than the cutoff recommended by the Intermountain Thoracic Society (ITS). The “mild” categories of restriction and obstruction are, therefore, also broader than recommended by ATS or ITS, and include “borderline” cases. The severe category of obstruction has a lower cutoff than given in the example by the ATS and includes patients with severe and very severe obstruction. Our definition of restriction includes patients with combined restrictive and obstructive defects. We define for completeness a category that includes isolated reduced Deo in absence of obstruction or restriction, and a category of reduced VC and/or FEV,, both without evidence for obstruction or restriction as defined in this article. canadian health & care mall
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Pulmonary Function Abnormalities
 For the 3PIT method, we used the iterative search procedure as described by Graham et al. The process started with a calculation of residual volume, RV = VA — IVC + VDS. Equations 6 (inspiration), 7 (breath hold), and 9 (expiration) of Graham et al were then used to iteratively calculate Deo. In equation 6, every 30 ms the measured incremental inspired volume (obtained from the recorded spirogram) was added to the lung volume, and the added CO and Ne were used to recalculate an instantaneous value for alveolar CO and Ne concentrations using gas dilution and diffusion equations. Inspired gas concentrations were assumed to equal concentrations in the inspired gas tank, obtained by chromatography prior to the first Deo maneuver in each patient. Equation 7 calculated the change in alveolar CO concentration during breath hold, assuming constant lung volume and uniform dilution of the inspired gas into the alveolar volume. Equation 9 calculated mean collected sample concentrations of Ne and CO using the recorded spirogram and gas diffusion equations to update lung volume and alveolar CO concentration every 30 ms. If the calculated CO concentration in the 500-ml alveolar sample (С О c) differed from the actual measured value ( С О m), then the Deo used in the diffusion equations was changed to Dco^ = Dcoo|d X [ С О J С О m + 1] X 2 where Dco^ and Dco^ are the values for Deo used in the previous and next iteration, respectively. The iterative calculation procedure started with a Deo value of 20 and iteration continued until Deo new differed from Dco(4d by less than 0.1 percent. Because gas chromatography measures wet gas concentrations, we adjusted the exhaled gas concentration to convert it to dry gas fraction, and during the calculation, all gas volumes were expressed as standard temperature and pressure, dry (STPD).
For the 3PIT method, we used the iterative search procedure as described by Graham et al. The process started with a calculation of residual volume, RV = VA — IVC + VDS. Equations 6 (inspiration), 7 (breath hold), and 9 (expiration) of Graham et al were then used to iteratively calculate Deo. In equation 6, every 30 ms the measured incremental inspired volume (obtained from the recorded spirogram) was added to the lung volume, and the added CO and Ne were used to recalculate an instantaneous value for alveolar CO and Ne concentrations using gas dilution and diffusion equations. Inspired gas concentrations were assumed to equal concentrations in the inspired gas tank, obtained by chromatography prior to the first Deo maneuver in each patient. Equation 7 calculated the change in alveolar CO concentration during breath hold, assuming constant lung volume and uniform dilution of the inspired gas into the alveolar volume. Equation 9 calculated mean collected sample concentrations of Ne and CO using the recorded spirogram and gas diffusion equations to update lung volume and alveolar CO concentration every 30 ms. If the calculated CO concentration in the 500-ml alveolar sample (С О c) differed from the actual measured value ( С О m), then the Deo used in the diffusion equations was changed to Dco^ = Dcoo|d X [ С О J С О m + 1] X 2 where Dco^ and Dco^ are the values for Deo used in the previous and next iteration, respectively. The iterative calculation procedure started with a Deo value of 20 and iteration continued until Deo new differed from Dco(4d by less than 0.1 percent. Because gas chromatography measures wet gas concentrations, we adjusted the exhaled gas concentration to convert it to dry gas fraction, and during the calculation, all gas volumes were expressed as standard temperature and pressure, dry (STPD).
Continue reading this post…
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Methods
Several technical abbreviations are used in the text (Table 1). Data were analyzed from diffusing capacity tests of patients referred to our outpatient pulmonary function testing laboratoiy. We did not screen the patients so that the patient population tested represents a typical sampling of patients referred to our laboratory for routine testing. The diffusing capacity was determined using an automated pulmonary function testing unit (Medical Graphics Corporation, St. Paul, Minn). When performing a test, the diffusion test gas mixture (0.3 percent CO, 0.5 percent Ne, 21 percent 02, and balance nitrogen) was first analyzed using a built-in gas chromatograph. Patients were instructed to exhale completely and then to rapidly inhale diffusion test gas and hold their breath for about 8 s. After breath hold, patients exhaled rapidly, during which the first 750 ml was discarded and the next 500 ml of expired gas was collected. In patients whose vital capacity was less than 2.0 L, the 500-ml sample was collected after 500 ml was expired. The expired gas sample was then drawn into the gas chromatograph for analysis of expired Ne and CO. Gas chromatography eliminates the need for a C02 correction.
Continue reading this post…
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method
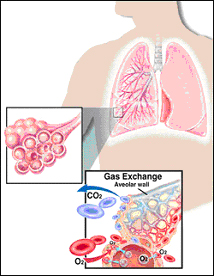
 The diffusing capacity of the lungs for carbon monoxide (Deo) can be estimated by a number of techniques, including steady state, single breath, and rebreathing. The single-breath method is most commonly used in the United States, probably because of better standardization and because it does not require a rapid CO analyzer. In the singlebreath method, patients are required to take a full vital capacity breath of the test gas mixture, hold their breath for about 10 s, then exhale. The equation used for calculation of diffusing capacity has breath-hold time in the denominator, where Deo is the diffusing capacity of the lungs for carbon monoxide, Va is the alveolar volume accessible to the inhaled test gas mixture, Pb is barometric pressure in mm Hg, Fa,x and Fi,x are the alveolar and inhaled concentrations of gases (carbon monoxide, CO, or Neon, Ne), IVC is the volume of inspired gas, and Vds is the sum of system (35 ml) and anatomic (150 ml) dead spaces. The initial alveolar CO concentration (Fa,co[0]) is calculated from Fi,co times a dilution factor (equation 3). All calculations are performed with gas volumes expressed STPD, though Va is reported in BTPS for comparison with plethysmographic TLC.
The diffusing capacity of the lungs for carbon monoxide (Deo) can be estimated by a number of techniques, including steady state, single breath, and rebreathing. The single-breath method is most commonly used in the United States, probably because of better standardization and because it does not require a rapid CO analyzer. In the singlebreath method, patients are required to take a full vital capacity breath of the test gas mixture, hold their breath for about 10 s, then exhale. The equation used for calculation of diffusing capacity has breath-hold time in the denominator, where Deo is the diffusing capacity of the lungs for carbon monoxide, Va is the alveolar volume accessible to the inhaled test gas mixture, Pb is barometric pressure in mm Hg, Fa,x and Fi,x are the alveolar and inhaled concentrations of gases (carbon monoxide, CO, or Neon, Ne), IVC is the volume of inspired gas, and Vds is the sum of system (35 ml) and anatomic (150 ml) dead spaces. The initial alveolar CO concentration (Fa,co[0]) is calculated from Fi,co times a dilution factor (equation 3). All calculations are performed with gas volumes expressed STPD, though Va is reported in BTPS for comparison with plethysmographic TLC.
Implicit assumptions underlying the calculations are (1) that the alveolar surface area available for diffusion is exposed to the inhaled gas mixture for the entire time of breath hold, and (2) there is both homogeneity in delivery of inspired gas to the entire Va and homogeneity of ratios of regional Deo to Va.2 These assumptions are not strictly valid and breath-hold time becomes an approximation of the time that the test gas mixture is exposed to the exchanging surface area. canadian neighborhood pharmacy
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Conclusion
Although the strength and endurance of the inspiratory muscles improved with training, the pulmonary function parameters, especially VC and 12s-MW, did not change. Similar effects were reported by Chen and coworkers and by Flynn and associates in patients with COPD during respiratory muscle training. Pulmonary function testing is known to be an insensitive parameter of inspiratory muscle function. The 12s-MW test is influenced by many factors and it may therefore fail to distinguish inspiratory muscle dysfunction from other causes for its impairment.
In our study, training not only improved diaphragmatic and global inspiratory muscle function, but nearly all of the adaptation gained from training Was also retained 6 months after the cessation of the training. Healthy young subjects who had 4 or 5 weeks of training lost at least 50 percent of the gain after 8 to 15 weeks of no training. Belman and Gaesser have shown in normal elderly subjects that almost all the adaptations gained from 8 weeks of training were retained 2 months after its cessation. It is therefore very likely that the adaptations in ventilatory muscles become greater with increased training period.
Continue reading this post…
