Category - Part 2
Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae: Data Collection
 Patients were excluded if their total hospitalization was < 2 days, if they had impaired immune function (ie, AIDS, HIV, leukocyte count < 1,000/^L), known or suspected tuberculosis, known or suspected Pneumocystis ji-roveci, or concomitant pneumonia or other infection at baseline caused by viruses, fungi, or other bacteria except intracellular pathogens (Mycoplasma pneumoniae, Chlamydophila pneumoniae, Legionella pneumoniae), Haemophilus influenzae, or Moraxella catarrhalis. naturalbreastenhancementpill.com
Patients were excluded if their total hospitalization was < 2 days, if they had impaired immune function (ie, AIDS, HIV, leukocyte count < 1,000/^L), known or suspected tuberculosis, known or suspected Pneumocystis ji-roveci, or concomitant pneumonia or other infection at baseline caused by viruses, fungi, or other bacteria except intracellular pathogens (Mycoplasma pneumoniae, Chlamydophila pneumoniae, Legionella pneumoniae), Haemophilus influenzae, or Moraxella catarrhalis. naturalbreastenhancementpill.com
Medical charts were reviewed for all identified patients, and data were collected using a standardized collection tool. Information documented included patient demographics; comorbid conditions (diabetes, COPD, neoplasm, congestive heart failure [CHF], cirrhosis, or other chronic liver disease); microbiology data including penicillin susceptibility and culture source; admission year; hospital length of stay; presence of ICU stay; pneumonia severity illness (PSI) score; antibiotic therapy (including route); daily maximum temperature and WBC count; and crude mortality at end of hospitalization.
Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae: Study Design
All can result in increased hospital length of stay, thereby significantly escalating costs. However, few cost-of-illness studies have attempted to evaluate the economic impact of penicillin susceptibility in patients with CAP caused by S pneumoniae. The primary objective of this study was to determine resource utilization and costs associated with the in-hospital treatment of CAP caused by S pneumoniae, as stratified by susceptibility to penicillin. A secondary objective was to determine other patient covariates that were predictive of a more costly hospital stay.
This was a retrospective cohort study of adult patients admitted to Hartford Hospital between 1999 and 2003 with documented CAP caused by S pneumoniae. Hartford Hospital is an 810-adult-bed, nonprofit, private, teaching hospital located in urban Hartford, CT. The institutional review board approved this study. Informed consent was not required since the study was retrospective in design and all protected health information was destroyed on completing data collection. Each patient received a subject number corresponding to a consecutively reviewed medical record and hospital bill. avandia online
Continue reading this post…
Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae
 Pneumonia is the sixth-leading cause of death in the United States and the number-one cause of death from an infectious disease. The subset of patients who acquire pneumonia while not residing in a hospital or long-term care facility for at least 2 weeks before the onset of symptoms are defined as having community-acquired pneumonia (CAP). Of the 4 to 5 million cases of CAP treated annually, a minority (approximately 0.5 to 1 million) are treated in a hospital. Yet, this minority has accounted for the majority of health-care costs associated with the infection; $8 billion was spent on hospitalization costs in 1994, compared with $0.4 billion spent among outpatients.
Pneumonia is the sixth-leading cause of death in the United States and the number-one cause of death from an infectious disease. The subset of patients who acquire pneumonia while not residing in a hospital or long-term care facility for at least 2 weeks before the onset of symptoms are defined as having community-acquired pneumonia (CAP). Of the 4 to 5 million cases of CAP treated annually, a minority (approximately 0.5 to 1 million) are treated in a hospital. Yet, this minority has accounted for the majority of health-care costs associated with the infection; $8 billion was spent on hospitalization costs in 1994, compared with $0.4 billion spent among outpatients.
Although most studies have been unable to identify the cause of CAP in approximately 50% of patients, the most common bacteria isolated in most reports have been Streptococcus pneumoniae. In a large metaanalysis of > 7,000 CAP cases, S pneumoniae accounted for two thirds of those for whom an etiologic diagnosis was made, as well as two thirds of the patients with bacteremic pneumonia.
Competition for Intrathoracic Space Reduces Lung Capacity in Patients With Chronic Heart Failure: Conclusion
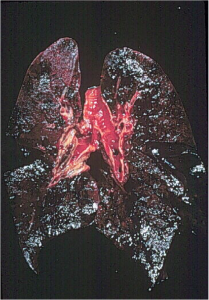 This muscle fiber atrophy is associated with significant reductions in tissue force generation, thus limiting resting tonality and potentially contributing the upward crescent shape of the diaphragm. Another potential contributor to the increased diaphragm volume includes ascites. Mutoh and col-leagues have shown, using a piglet model, a 40% reduction in TLC as a result of increased abdominal volume through a surgically implanted water-filled balloon. Although this relationship has yet to be fully examined in humans, the majority of the heart failure patients in the present study were clinically stable and did not have apparent ascites or otherwise significant abdominal distension.
This muscle fiber atrophy is associated with significant reductions in tissue force generation, thus limiting resting tonality and potentially contributing the upward crescent shape of the diaphragm. Another potential contributor to the increased diaphragm volume includes ascites. Mutoh and col-leagues have shown, using a piglet model, a 40% reduction in TLC as a result of increased abdominal volume through a surgically implanted water-filled balloon. Although this relationship has yet to be fully examined in humans, the majority of the heart failure patients in the present study were clinically stable and did not have apparent ascites or otherwise significant abdominal distension.
Importantly, a potential limitation to this study is the use of a single equation to estimate pulmonary blood and parenchymal tissue volumes in control subjects and patients with chronic heart failure. Understandably, the use of a single prediction equation may have a tendency to slightly underestimate actual volumes in this population. Until recently, pulmonary fluid accumulation was thought to be a chronic process occurring as a result of cardiac contractile insufficiency leading to elevated left atrial pressure, increased pulmonary venous pressure, and concomitant distension of the pulmonary vasculature, coupled with generalized central and peripheral fluid accumulation and retention. buy birth control pills online
Competition for Intrathoracic Space Reduces Lung Capacity in Patients With Chronic Heart Failure: Results
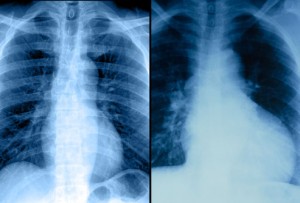 The relationship between NYHA class and absolute lung volume and percentage of TTCV that is taken up by the lung is shown in Figure 3, top, A, and bottom, B, respectively. These data suggest a clear relationship between increasing NYHA class and elevated cardiac volume and reduction in lung volume. Figure 4 demonstrates the close correlation (r = — 0.81, p < 0.001) between elevated cardiac size and reduction in lung volume within the entire population separated by groups. In this study, we found the following in patients with heart failure compared to control participants: (1) marked increases in cardiac size reaching twice that of healthy age- and gender-matched control participants; (2) a clear relationship between the severity of heart failure and increase in cardiac size; (3) and a negative correlation between the percentage of TTC occupied by lung and the percentage of TTC occupied by the heart. add comment
The relationship between NYHA class and absolute lung volume and percentage of TTCV that is taken up by the lung is shown in Figure 3, top, A, and bottom, B, respectively. These data suggest a clear relationship between increasing NYHA class and elevated cardiac volume and reduction in lung volume. Figure 4 demonstrates the close correlation (r = — 0.81, p < 0.001) between elevated cardiac size and reduction in lung volume within the entire population separated by groups. In this study, we found the following in patients with heart failure compared to control participants: (1) marked increases in cardiac size reaching twice that of healthy age- and gender-matched control participants; (2) a clear relationship between the severity of heart failure and increase in cardiac size; (3) and a negative correlation between the percentage of TTC occupied by lung and the percentage of TTC occupied by the heart. add comment
Competition for Intrathoracic Space Reduces Lung Capacity in Patients With Chronic Heart Failure: Statistical Analysis
Statistical analysis and graphic presentation were accomplished using statistical software (Prism version 4.0; Graphpad; San Diego, CA). One-way analysis of variance was used to test for differences in means among the groups, and unpaired t test was used to compare the means of the participant characteristics and radiographic variables between the control and chronic heart failure groups and between chronic heart failure groups. Pearson correlation coefficients were calculated between radiographic measures and measures of heart failure severity. Fisher Exact Test was used to examine the difference in medication usage and other categorical variables between groups. Statistical significance was set at p < 0.05 for all analyses. Data are presented as mean ± SD or number and percentage of the group, as appropriate.
Continue reading this post…
Competition for Intrathoracic Space Reduces Lung Capacity in Patients With Chronic Heart Failure: Population Characteristics
 The TTC volume (TTCV) was determined as follows: (1) the posteroanterior and lateral view-digitized tracings were divided vertically into five sections, with the upper two sections equally divided into 2.75-cm segments, and the third and fourth sections equally divided between the most superior border of the diaphragm and lower border of the second section; (2) the fifth section included the region from the dome of the diaphragm to the insertion of the diaphragm with the rib cage; (3) and the volume of each elliptical cylindroid was calculated using the following formula:
The TTC volume (TTCV) was determined as follows: (1) the posteroanterior and lateral view-digitized tracings were divided vertically into five sections, with the upper two sections equally divided into 2.75-cm segments, and the third and fourth sections equally divided between the most superior border of the diaphragm and lower border of the second section; (2) the fifth section included the region from the dome of the diaphragm to the insertion of the diaphragm with the rib cage; (3) and the volume of each elliptical cylindroid was calculated using the following formula:
TTCV = (1/4то) X Dx X D2 X D3
where D1 is the width across the posteroanterior view, D2 is the depth from the lateral view, and D3 is the height of the posteroanterior view. Total thoracic volume was defined as the sum of each of the individual segment volumes (Fig 1). in detail
Total cardiac volume was calculated using the following formula:
cardiac volume = (1/6to) X Dj X D2 X D3
where D1 is the long diameter measured by establishing the longest line from the junction of the superior venous pedicle with the right atrium to the apex of the left ventricle from the posteroanterior view of the cardiac silhouette, D2 is the transverse diameter defined as the sum of two perpendicular lines extended from D1 to the furthest points of the left and right ventricular borders, and D3 is the depth of the cardiac silhouette defined as the longest diameter on the lateral view approximately perpendicular to D1 (Fig 1).
Continue reading this post…
