Category - Part 8
Diffusing Capacity for Nitric Oxide and Carbon Monoxide in Patients With Diffuse Parenchymal Lung Disease and Pulmonary Arterial Hypertension: Dlno Measurement
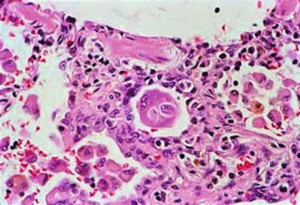 All patients with suspected PAH underwent radionuclide perfusion and ventilation scans, echocardiography with estimation of the pulmonary artery pressure by tricuspid regurgitation measurement (assessed by experienced cardiologists), CT scan of the pulmonary arteries in order to detect central thromboembolic disease, right heart catheterization with measurements of the pulmonary artery pressure with reversibility testing in most patients (epoprostenol), and pulmonary angiography when indicated. Consultation by rheumatologists included the performance of serum immunologic tests in search of collagen vascular disease and scleroderma. A definite diagnosis of PAH was made based on the Revised Clinical Classification of Pulmonary Hypertension. further
All patients with suspected PAH underwent radionuclide perfusion and ventilation scans, echocardiography with estimation of the pulmonary artery pressure by tricuspid regurgitation measurement (assessed by experienced cardiologists), CT scan of the pulmonary arteries in order to detect central thromboembolic disease, right heart catheterization with measurements of the pulmonary artery pressure with reversibility testing in most patients (epoprostenol), and pulmonary angiography when indicated. Consultation by rheumatologists included the performance of serum immunologic tests in search of collagen vascular disease and scleroderma. A definite diagnosis of PAH was made based on the Revised Clinical Classification of Pulmonary Hypertension. further
Diffusing Capacity for Nitric Oxide and Carbon Monoxide in Patients With Diffuse Parenchymal Lung Disease and Pulmonary Arterial Hypertension: Patients
Assuming that the Dlno is not affected or is less affected by impaired capillary filling, and thus represents the diffusing capacity of the pulmonary membrane, the Dlno/Dlco ratio has to differ between subjects with a pure alveolocapillary membrane disturbance and subjects with microvascular disease. Subjects with a decreased Dlco due to lowering of the Vcap component will have undisturbed Dlno; therefore, the Dlno/Dlco ratio will increase. Subjects with a decreased Dlco due to thickening of the membrane without disturbing the pulmonary capillaries will also have a lower Dlno, so the Dlno/Dlco ratio will not alter. The study by Harris et al7 demonstrated in sheep that the occlusion of one pulmonary artery increased the Dlno/ Dlco ratio by decreasing the Dlco while the Dlno remained constant. This effect is caused by the increase in CO backpressure in stagnant capillaries. The authors concluded that the Dlco has a much greater sensitivity than Dlno in detecting a regional reduction in capillary blood flow. The aim of this study was to test the hypothesis that the Dlno/ Dlco ratio significantly differs between patients with diffusion impairment due to fibrotic disease and patients with diffusion impairment due to pulmonary vascular disease.
Diffusing Capacity for Nitric Oxide and Carbon Monoxide in Patients With Diffuse Parenchymal Lung Disease and Pulmonary Arterial Hypertension
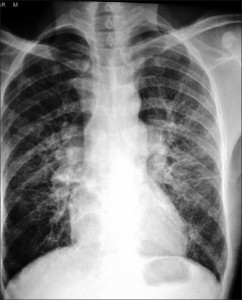 The diffusing capacity of the lung for carbon monoxide (Dlco) estimates the amount of gas uptake by the lungs and is a valuable tool in the assessment of pulmonary diseases. According to the model of Roughton and Forster, Dlco is determined by the following several factors: the passage of carbon monoxide (CO) through the alveolocapillary membrane; the transfer of CO into the plasma and the intraerythrocytic compartments; and the reaction rate for the binding of CO on hemoglobin (Hb). Equation 1 enables the estimation of the two components of the Dlco (ie, the diffusing capacity of the alveolocapillary membrane for CO [Dmco] and the pulmonary capillary blood volume [Vcap]) using duplicate measurements of the Dlco with high and low oxygen concentrations.
The diffusing capacity of the lung for carbon monoxide (Dlco) estimates the amount of gas uptake by the lungs and is a valuable tool in the assessment of pulmonary diseases. According to the model of Roughton and Forster, Dlco is determined by the following several factors: the passage of carbon monoxide (CO) through the alveolocapillary membrane; the transfer of CO into the plasma and the intraerythrocytic compartments; and the reaction rate for the binding of CO on hemoglobin (Hb). Equation 1 enables the estimation of the two components of the Dlco (ie, the diffusing capacity of the alveolocapillary membrane for CO [Dmco] and the pulmonary capillary blood volume [Vcap]) using duplicate measurements of the Dlco with high and low oxygen concentrations.
Continue reading this post…
Discriminating Measures and Normal Values for Expiratory Obstruction: Recommendation
There are several possible limitations in this study. Although the spirometric measurements followed ATS guidelines, it is possible that some subjects gave incomplete historical details. While we do not have data for Asian individuals or other ethnic groups, the similarity of FEV1/FVC and FEV3/FVC values among thousands of white, black, and Latin adults in the United States, who differed considerably in height and nutritional status, suggests that the values given in Table 4 are likely to be universally valid. In clinical practice, we would express uncertainty when spirometric findings are equivocal, but purposely did not do so in this study. Rather, we distinguished normalcy from abnormality on purely statistical grounds, as have other authors.- The use of a single-tailed LLN at the 95% confidence level in a healthy population causes approximately 5% of each measurement to be “abnormal,” although the subject may not really be abnormal.
Discriminating Measures and Normal Values for Expiratory Obstruction: Conclusion
 In evaluating the cigarette-smoking effect in the NHANES III population, both the decreases in FEV1/FVC and increases in 1 — FEV3/FVC for a given age group are striking (Fig 3). Using either measurement, fractions progressively deteriorate with age relative to the never-smoking subjects. Consequently, by middle age current smokers have similar values to those of never-smokers who are about 20 years older (Fig 3). In both our study (Table 3) and that of Miller et al, abnormal FEV3/FVC values were as common as abnormal FEV1/FVC values. This suggests that attention similar to that accorded to FEV1/FVC should be paid to FEV3/FVC and 1 — FEV3/FVC in evaluating airway obstruction. Because values for both FEV1/FVC and FEV3/FVC normally decline at a relatively constant rate with aging, using fixed ratios such as 70% or 73% for FEV1/FVC or any other value for FEV3/FVC as the mean or LLN values should be avoided. www.canadian-familypharmacy.com
In evaluating the cigarette-smoking effect in the NHANES III population, both the decreases in FEV1/FVC and increases in 1 — FEV3/FVC for a given age group are striking (Fig 3). Using either measurement, fractions progressively deteriorate with age relative to the never-smoking subjects. Consequently, by middle age current smokers have similar values to those of never-smokers who are about 20 years older (Fig 3). In both our study (Table 3) and that of Miller et al, abnormal FEV3/FVC values were as common as abnormal FEV1/FVC values. This suggests that attention similar to that accorded to FEV1/FVC should be paid to FEV3/FVC and 1 — FEV3/FVC in evaluating airway obstruction. Because values for both FEV1/FVC and FEV3/FVC normally decline at a relatively constant rate with aging, using fixed ratios such as 70% or 73% for FEV1/FVC or any other value for FEV3/FVC as the mean or LLN values should be avoided. www.canadian-familypharmacy.com
Discriminating Measures and Normal Values for Expiratory Obstruction: Discussion
Two prior studies have given reference values for FEV3/FVC. Each study used 200 to 300 nonsmoking white adults of northern European ethnicity. Over a broad age and height range, our mean FEV3/FVC values for white never-smokers are, on average, approximately 1.7% and 1.0% lower than those for men and women reported in the study by Crapo et al and < 1% lower than those reported in the study by Miller et al.> These small differences may relate to resident altitudes, socioeconomic factors, or other unknown factors. Although Miller et al did not emphasize the following information, their data from 359 current smokers showed that FEV3/FVC abnormalities exceeded those of FEV1/ FVC, FEF50, FEF25-75, FEV1, FEV3, FEF75, and flow between 75% and 85% of the FVC (FEF75-85). in detail
In a consensus statement from the National Lung Health Education Program, Ferguson et al reported that 9.6% of the adult (ie, 18 to 89 years of age) NHANES III smokers had an obstructive pattern, which they defined as FEV1/FEV6 and FEV1 values below the LLN. In our series of 3,570 current smokers, aged 20 to 80 years, a considerably larger percentage (Table 3) showed airflow limitation as manifested by significant decreases in FEV1/FVC and FEV3/FVC.
Continue reading this post…
Discriminating Measures and Normal Values for Expiratory Obstruction: Results
 A total of 1,167 (ie, the sum of values from lines b to n, Table 3) of 3,570 smokers had abnormal patterns. Eight hundred one smokers had expiratory obstruction; 66% of smokers (530 of 801 smokers) [lines d to f, Table 3] had both early and late expiratory obstruction with or without possible restriction; 16% of smokers (130 of 801 smokers) [lines g to i, Table 3] had late expiratory obstruction with or without possible restriction; and 18% of smokers (141 of 801 smokers) [lines j to l, Table 3] had early expiratory obstruction with or without possible restriction. www.canadian-familypharmacy.com
A total of 1,167 (ie, the sum of values from lines b to n, Table 3) of 3,570 smokers had abnormal patterns. Eight hundred one smokers had expiratory obstruction; 66% of smokers (530 of 801 smokers) [lines d to f, Table 3] had both early and late expiratory obstruction with or without possible restriction; 16% of smokers (130 of 801 smokers) [lines g to i, Table 3] had late expiratory obstruction with or without possible restriction; and 18% of smokers (141 of 801 smokers) [lines j to l, Table 3] had early expiratory obstruction with or without possible restriction. www.canadian-familypharmacy.com
Many smokers with expiratory obstruction had probable false-negative FEF25-75 test results. A total of 683 smokers (lines d, e, g, h, j, and k, Table 3) had expiratory obstruction but without restriction, 42% of whom (287 of 683 smokers) had normal and probable false-negative FEF25-75 test results. These results included 40% of smokers (114 of 268 smokers) with both abnormal FEV1/FVC and FEV3/FVC values (line d, Table 3) and 84% of smokers (90 of 107 smokers) with abnormal FEV3/FVC values (line g), with both groups being older (mean ages, 59 and 54 years, respectively). But, 64% of smokers (67 of 104 smokers) [line j, Table 3] with abnormal FEV1/ FVC values with normal and probable false-negative FEF25-75 test results tended to be younger. Thus, measurements of FEF25-75 especially in older individuals, often disagree with other spirometric measurements with less inherent variability.
Continue reading this post…
