Latest News - Part 34
Outcome of Patients Requiring Medical ICU Admission Following Bone Marrow Transplantation: Results
There were 229 BMTs performed at our institution (129 allogeneic transplants and 100 autologous transplants) between March 3, 1984 and March 26, 1991. During this period 36 of these patients (15.7 percent) had 43 admissions to the MICU. The admission data for these patients in terms of outcome are summarized in Table 1.
There was no statistically significant difference in age between the survivors and nonsurvivors, 34.4 years vs 37.6 years of age, respectively. Of these patients, 19 were male and 17 were female. The indications for BMT included acute myeloid leukemia in 14, lymphoma in 10, chronic myelogenous leukemia in 6, acute lymphocytic leukemia in 4, aplastic anemia in 1, and small-cell carcinoma of the lung in 1. There was no statistically significant difference in outcome with regard to the patients indication for BMT. A larger percentage of nonsurvivors had disease in remission, but this trend was not statistically different. Similarly, there was no statistically significant difference in outcome between the 28 patients who had allogeneic transplants and the 8 patients who had autologous transplants. Furthermore, we did not determine a difference in outcome with regard to a patients conditioning regimen. Of those patients with GVHD, 82 percent did not survive, but this difference was not statistically different when compared with those without GVHD.
Continue reading this post…
Outcome of Patients Requiring Medical ICU Admission Following Bone Marrow Transplantation: Methods
 Over the past two decades, bone marrow transplantation (BMT) has become accepted as a standard treatment modality in adults with aplastic anemia (AA), acute lymphocytic leukemia (ALL), acute myeloid leukemia (AML), chronic myelogenous leukemia (CML), lymphoma, and certain solid tumors. Prior to BMT, patients receive conditioning regimens that include myeloablative chemotherapy often accompanied by total-body irradiation. For at least 2 weeks after BMT, patients will experience profound leuko-cytopenia and thrombocytopenia. This and the additional use of immunosuppressive therapy place these patients at increased risk for numerous complications, including opportunistic infections, bleeding, and graft-vs-host disease (GVHD).
Over the past two decades, bone marrow transplantation (BMT) has become accepted as a standard treatment modality in adults with aplastic anemia (AA), acute lymphocytic leukemia (ALL), acute myeloid leukemia (AML), chronic myelogenous leukemia (CML), lymphoma, and certain solid tumors. Prior to BMT, patients receive conditioning regimens that include myeloablative chemotherapy often accompanied by total-body irradiation. For at least 2 weeks after BMT, patients will experience profound leuko-cytopenia and thrombocytopenia. This and the additional use of immunosuppressive therapy place these patients at increased risk for numerous complications, including opportunistic infections, bleeding, and graft-vs-host disease (GVHD).
Pulmonary complications have been observed in 40 to 60 percent of patients with BMTs. These include interstitial pneumonitis in up to 40 percent of allogeneic BMT recipients, bacterial, viral, and fungal pneumonias, cardiogenic and noncardiogenic pulmonary edema, bronchiolitis obliterans, and alveolar hemorrhage syndrome. With these severe acute complications, it has been estimated that 30 to 40 percent of BMT recipients require treatment.
Continue reading this post…
Maximal Inspiratory Pressure: Test-Retest Reliability
 Performance did not technically plateau, but systematic differences between Pimax measured at the third and fourth test sessions were very small; hence, data from these sessions were examined for test-retest reliability. The mean absolute difference, cumulative frequency distribution for the absolute difference, and the 95 percent confidence interval for the absolute difference indicated that Pimax fluctuated by approximately 5 cm HzO or less in most of the sample. This was consistent with other measures of strength where day-to-day fluctuations were reported to be ± 10 percent. However, a portion of the sample demonstrated wider fluctuations. Taking a conservative approach, we conclude that when monitoring individual patients at repeated intervals, Pimax must change by approximately 10 cm H20 or more before it can be interpreted as a clinical change in strength. Moreover, a repeatable trend must be established to confirm a change in strength.
Performance did not technically plateau, but systematic differences between Pimax measured at the third and fourth test sessions were very small; hence, data from these sessions were examined for test-retest reliability. The mean absolute difference, cumulative frequency distribution for the absolute difference, and the 95 percent confidence interval for the absolute difference indicated that Pimax fluctuated by approximately 5 cm HzO or less in most of the sample. This was consistent with other measures of strength where day-to-day fluctuations were reported to be ± 10 percent. However, a portion of the sample demonstrated wider fluctuations. Taking a conservative approach, we conclude that when monitoring individual patients at repeated intervals, Pimax must change by approximately 10 cm H20 or more before it can be interpreted as a clinical change in strength. Moreover, a repeatable trend must be established to confirm a change in strength.
Continue reading this post…
Maximal Inspiratory Pressure: Discussion
The mean Pimax was consistent with values reported for similar groups of patients with moderate to severe COPD. The results of this study supported the notion that in naive COPD patients, performance of Pimax improves with practice of the Pimax maneuver. The third and fourth test of Pimax produced reliable data.
Learning Effect
Systematic differences between consecutive tests were relatively small but at the fourth test, Pimax was 17 percent higher than at the first test. Other investigators observed similar increases in Pimax during an initial learning period, but for most the observed improvements in Pimax were not statistically significant because they used smaller samples with inadequate statistical power to detect an effect of this magnitude. The study of Ringquist2 is the one exception. He studied a larger sample and found no statistically significant improvement with the second measure of Pimax. This apparent inconsistency with our results may be attributed to the number of trials employed with each test session and the level of motivation. Ringquist2 studied healthy military conscripts who were highly motivated and athletic as compared with our COPD patients. Moreover, he conducted approximately ten trials per session, whereas we conducted five trials. It is possible that the high level of motivation and the additional number of trials enabled subjects to learn the Pimax maneuver in a single session.
Continue reading this post…
Maximal Inspiratory Pressure: Results
 The sample was 69 men and 22 women with moderate to severe COPD (Table 1). Most patients were taking standard pharmacologic therapies, including inhaled p-agonists, oral (3-agonists, and methylxan-thines. Nine were using home oxygen. Ten were currently smoking, one had never smoked, and the remainder had quit smoking. The sample was middle class as indicated by the Hollingshead Index.
The sample was 69 men and 22 women with moderate to severe COPD (Table 1). Most patients were taking standard pharmacologic therapies, including inhaled p-agonists, oral (3-agonists, and methylxan-thines. Nine were using home oxygen. Ten were currently smoking, one had never smoked, and the remainder had quit smoking. The sample was middle class as indicated by the Hollingshead Index.
Performance gradually improved as demonstrated by the mean (SD) Pimax for each test session: first — 53 (24) cm H20, second -57 (25) cm H20, third -60 (25) cm H20, and fourth -62 (25) cm H20. Analysis of variance for repeated measures identified a significant increase in Pimax with a significant linear effect and no significant curvilinear effect over time (p<0.001). Statistically, performance did not plateau; however, between the third and fourth tests, the net increase in Pimax was so small that it was not clinically significant and performance appeared to be plateauing (Table 2). The frequency distribution for net differences in Pimax is presented in Figure 1. A weak negative correlation between Pimax and age was strengthened from the first (r= —19; p>0.05) to the fourth test session (r= —0.30; p<0.01).
Continue reading this post…
Maximal Inspiratory Pressure: Data Analysis
The Pimax was defined as the largest negative pressure generated at the mouth and maintained for at least 1 full second. A minimum of five technically satisfactory trials were conducted for each test and data w^ere discarded if there was an air leak around the mouthpiece or if the pressure was held for less than 1 full second as estimated by the data collector. The initial length of the inspiratory muscles wras controlled by initiating each effort from residual volume (RV). This procedure was adopted because in the clinical situation RV is more reproducible than functional residual capacity (FRC). Patients were instructed to take their time and slow ly empty their lungs to RV, thereby avoiding problems associated with variability in lung volumes caused by dynamic hyperinflation. Patients were not allowed to view the gauge during testing.
Data were collected by two researchers who were experienced in conducting these tests. Tests were conducted in a quiet room with no distractions and the same instructions were given to patients at the beginning of each testing session. Patients were coached in a consistent manner during each maximal inspirator)’ effort and brief rest periods of slightly less than 1 min were taken between repeated Pimax trials. Patients were instructed to take their time and indicate when they were ready to perform each maneuver. Test sessions were conducted at the same time of day and by the same researcher for each patient. Patients were instructed to take their usual medications as scheduled on each day of testing to control for any potential drug effects on respiratory muscle function.
Continue reading this post…
Maximal Inspiratory Pressure: Method
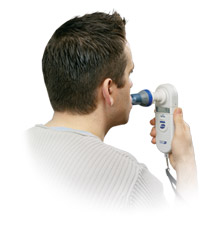
 Maximal inspiratory pressure (Pimax) is commonly used to measure inspiratory muscle strength. It reflects the force-generating ability of the combined inspiratory muscles during a brief quasi-static contraction.
Maximal inspiratory pressure (Pimax) is commonly used to measure inspiratory muscle strength. It reflects the force-generating ability of the combined inspiratory muscles during a brief quasi-static contraction.
The Pimax test is simple to perform and usually measured during a single test session with several trials. However, reliability has not been fully addressed in the research literature, specifically with respect to quantifying systematic measurement error associated with learning effects and day-to-day fluctuations associated with technical and/or methodologic errors and biologic variability in performance. Several studies examined the issue and most reported high test-retest reliabilities for repeated measures and no significant increase in Pimax with repeated measurements in naive subjects. However, in most studies, reliability was described on the basis of two or three test sessions, making it difficult to separate the systematic measurement error associated with learning effects from the day-to-day fluctuations in performance.
We examined initial learning effects and test-retest reliability of Pimax as measured at four test sessions in patients with COPD using a method that can be easily employed in the office or clinic setting.
Continue reading this post…

 Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.
Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.