Latest News - Part 29
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission: Statistical Analysis
 Study Design
Study Design
The subjects came to the laboratory on three different occasions. On the first visit, one of the investigators administered a questionnaire on the characteristics of their former asthma (duration, severity, medication requirements, potential initiating factors, time of asthma diagnosis and of remission, including last 2 years’ respiratory symptoms, and family history of asthma). Lung volumes, expiratory flows, and bronchodilator response were measured. Skin prick tests with 26 common airborne allergens completed this first visit.
Measurements
The subjects were asked to measure their peak expiratory flow rates (PEFRs) with a peak flow meter (mini-Wright) twice daily for a 2-week period. They recorded on a diary card the results of three reproducible PEFR measurements in the morning and in the evening. Pulmonary function tests included three reproducible measurements of FEVi and forced vital capacity (FVC) before and after inhalation of albuterol (200 fig). Measurements were obtained with a spirometer (Vitalograph PTF II). Pulmonary volumes were measured by body plethysmography according to the method of Dubois et al. canadian neightbor pharmacy
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission: Methods
Subjects
Sixty-five subjects took part in this study (Table 1). Of these, 30 ex-asthmatics were recruited from advertisements in different media.
Inclusion Criteria and Definition of Asthma Remission
We included in the study men or women >18 years old, atopic or not, with a proven history of asthma responding to the American Thoracic Society criteria, who were considered to be in asthma remission for at least 2 years. “Remission” of asthma was defined according to the definitions of Bronnimann and Burrows: “asthma was considered to be inactive (ex-asthma) if the subject denied medications, asthmatic attacks, and ‘frequent’ (more than two) attacks of shortness of breath with wheezing during the preceding year.” We, however, extended the minimum period of symptom remission to 2 years, to be included in the study.
We considered that our subjects had “proven asthma” according to the following criteria: all had a history of dyspnea and wheezing in the past; 26 subjects had a diagnosis of asthma made by a physician; 16 had previous available chart recordings of typical asthma presentation and wheezing on chest auscultation; 27 had used antiasthma medications (mostly bronchodilators) for different periods of time; and physiologic data showing airflow obstruction were available in 10 subjects. Furthermore, ten subjects had been hospitalized previously for their asthma and five had required mechanical ventilation for acute asthma.
Continue reading this post…
Persistence of Airway Obstruction and Hyperresponsiveness in Subjects With Asthma Remission
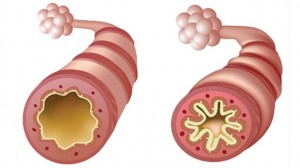 Bronchial asthma is characterized by variable airflow obstruction and airway hyperresponsiveness. Its underlying mechanism is considered to be an airway inflammatory process with bronchial epithelial damage and mucus secretion, and in which eosinophils and lymphocytes seem to play a key role.2 There is still no cure for asthma. We may, however, observe remissions, either spontaneously, after withdrawal of exposure to a sensitizing agent, or following bronchial anti-inflammatory therapy. Remissions are mostly observed in children, being quite rare in adults. Relapses of asthma after remission, however, are frequent in children. Blair reported a 20 percent recurrence of wheezing after a period of 3 years without symptoms in asthmatic children. Ryssing reported that in 36 percent of asthmatics who remitted from their asthma, wheezing resumed after a 13-year follow-up. In another study, 31 percent of young adults free of wheezing at 21 years old had recurrent wheezing at 28 years. mycanadianpharmacy.com
Bronchial asthma is characterized by variable airflow obstruction and airway hyperresponsiveness. Its underlying mechanism is considered to be an airway inflammatory process with bronchial epithelial damage and mucus secretion, and in which eosinophils and lymphocytes seem to play a key role.2 There is still no cure for asthma. We may, however, observe remissions, either spontaneously, after withdrawal of exposure to a sensitizing agent, or following bronchial anti-inflammatory therapy. Remissions are mostly observed in children, being quite rare in adults. Relapses of asthma after remission, however, are frequent in children. Blair reported a 20 percent recurrence of wheezing after a period of 3 years without symptoms in asthmatic children. Ryssing reported that in 36 percent of asthmatics who remitted from their asthma, wheezing resumed after a 13-year follow-up. In another study, 31 percent of young adults free of wheezing at 21 years old had recurrent wheezing at 28 years. mycanadianpharmacy.com
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Conclusion
 Our results with the 3PIT method can be only loosely compared with results of Graham et al who documented the differences in Deo using Og, JM, ESP, and three-equation methods in patients with emphysema, asthma, and cystic fibrosis. For both Og and JM methods, Graham et al allowed a 1-L dead space washout volume and collected a 1-L gas sample, whereas we used either a 750-ml (VC > 2.0 L) or 500-ml (VC < 2.0 L) dead space washout volume and a 500-ml gas sample. In the three-equation method, Graham et al used the entire expired volume in the computation whereas we were limited to the 500-ml gas sample that was collected by the automated equipment. They found that the ESP method gave the largest calculated Deo compared with Og, JM, and three-equation Deo in patients with emphysema or cystic fibrosis, and 4 percent larger than three-equation Deo in patients with asthma. The pulmonary function abnormalities in our 46 patients with Og > 3PIT included restriction, obstruction, isolated low Deo and reduced FVC and FEVr Graham et al did not state the severity of obstruction in their patient groups, nor did they document differences in Deo by the various methods in patients with pulmonary function abnormalities other than airflow limitation.
Our results with the 3PIT method can be only loosely compared with results of Graham et al who documented the differences in Deo using Og, JM, ESP, and three-equation methods in patients with emphysema, asthma, and cystic fibrosis. For both Og and JM methods, Graham et al allowed a 1-L dead space washout volume and collected a 1-L gas sample, whereas we used either a 750-ml (VC > 2.0 L) or 500-ml (VC < 2.0 L) dead space washout volume and a 500-ml gas sample. In the three-equation method, Graham et al used the entire expired volume in the computation whereas we were limited to the 500-ml gas sample that was collected by the automated equipment. They found that the ESP method gave the largest calculated Deo compared with Og, JM, and three-equation Deo in patients with emphysema or cystic fibrosis, and 4 percent larger than three-equation Deo in patients with asthma. The pulmonary function abnormalities in our 46 patients with Og > 3PIT included restriction, obstruction, isolated low Deo and reduced FVC and FEVr Graham et al did not state the severity of obstruction in their patient groups, nor did they document differences in Deo by the various methods in patients with pulmonary function abnormalities other than airflow limitation.
Continue reading this post…
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Discussion
Our main findings are as follows: (1) the singlebreath Deo was largest using the ESP timing method compared with JM, 3PIT, and Og methods (in decreasing order of mean Deo); (2) the difference between Deo using Og, JM, and 3PIT methods was small in patients with normal pulmonary function and became less in patients with obstruction, restriction, or low Deo; and (3) the reproducibility of Deo for replicate maneuvers was equivalent among the four methods. The differences among JM, Og and ESP timings reside in differences in definition of start and end of breath hold (Fig 1). Using backward elimination of nonsignificant terms, only IT and ET remained a significant term in the multiple regression models comparing Deo by Og, ESP, and JM (Table 4). The ESP gives the largest Deo in all patient groups because it uses the shortest breath hold time, start of breath hold being generally later than Og and JM, and end of breath hold at beginning of sampling. The Og is smallest in patients with normal expiratory flows because the Og inspiratory time is always larger than the others, due to the earlier start of breath hold. In normal individuals the differences between JM and both Og and ESP definitions for end of breath hold were insignificant. canadianneighborpharmacy.com
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Results
 The mean percents of predicted values for pulmonary function variables are listed in Table 2, categorized by pulmonary function abnormalities. Mean and SD values for Deo and the mean WP-SD of Deo by the various protocols are listed in Table 3 using the same categorization. The ESP protocol resulted in the largest Deo, followed by the JM and 3PIT methods, with Og resulting in the smallest Deo in most categories. The differences among Deo by various timing methods was significant (p < 0.01) for all paired comparisons in the group with normal patterns of pulmonary function. In other categories, the differences were generally less, and statistical significance was not attained in a number of comparisons. The JM and 3PIT Dcos were not significantly different in moderate to severe obstruction, restriction, or reduced Deo patient groups. The JM was less than ESP Deo in all patient groups except moderate restriction and isolated reduced Deo. The Og remained significantly less than JM, ESP, and 3PIT Dcos in all groups except in the moderate restriction and reduced Deo groups, where Og and 3PIT Dcos were not significantly different. The intrasubject SD of Deo was generally not significantly different among groups (p > 0.01) with the exception of the 3PIT method that gave the least reproducible Deo in the group with mild restriction. buy tavist online
The mean percents of predicted values for pulmonary function variables are listed in Table 2, categorized by pulmonary function abnormalities. Mean and SD values for Deo and the mean WP-SD of Deo by the various protocols are listed in Table 3 using the same categorization. The ESP protocol resulted in the largest Deo, followed by the JM and 3PIT methods, with Og resulting in the smallest Deo in most categories. The differences among Deo by various timing methods was significant (p < 0.01) for all paired comparisons in the group with normal patterns of pulmonary function. In other categories, the differences were generally less, and statistical significance was not attained in a number of comparisons. The JM and 3PIT Dcos were not significantly different in moderate to severe obstruction, restriction, or reduced Deo patient groups. The JM was less than ESP Deo in all patient groups except moderate restriction and isolated reduced Deo. The Og remained significantly less than JM, ESP, and 3PIT Dcos in all groups except in the moderate restriction and reduced Deo groups, where Og and 3PIT Dcos were not significantly different. The intrasubject SD of Deo was generally not significantly different among groups (p > 0.01) with the exception of the 3PIT method that gave the least reproducible Deo in the group with mild restriction. buy tavist online
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Standard Deviation
Predicted values were taken from Miller et al for Deo and TLC, and Miller for FVC and FEV,. Standing height (cm) without shoes and weight (kg) were measured immediately prior to pulmonary function evaluation. These categories are used as a framework within which to illustrate the dependence of the differences among Deo values on pulmonary function abnormality. The “normal” category is narrowly defined, with a higher cutoff than the example given by the ATS and probably higher than the cutoff recommended by the Intermountain Thoracic Society (ITS). The “mild” categories of restriction and obstruction are, therefore, also broader than recommended by ATS or ITS, and include “borderline” cases. The severe category of obstruction has a lower cutoff than given in the example by the ATS and includes patients with severe and very severe obstruction. Our definition of restriction includes patients with combined restrictive and obstructive defects. We define for completeness a category that includes isolated reduced Deo in absence of obstruction or restriction, and a category of reduced VC and/or FEV,, both without evidence for obstruction or restriction as defined in this article. canadian health & care mall

 Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.
Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.