Latest News - Part 30
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Pulmonary Function Abnormalities
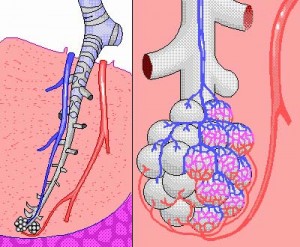 For the 3PIT method, we used the iterative search procedure as described by Graham et al. The process started with a calculation of residual volume, RV = VA — IVC + VDS. Equations 6 (inspiration), 7 (breath hold), and 9 (expiration) of Graham et al were then used to iteratively calculate Deo. In equation 6, every 30 ms the measured incremental inspired volume (obtained from the recorded spirogram) was added to the lung volume, and the added CO and Ne were used to recalculate an instantaneous value for alveolar CO and Ne concentrations using gas dilution and diffusion equations. Inspired gas concentrations were assumed to equal concentrations in the inspired gas tank, obtained by chromatography prior to the first Deo maneuver in each patient. Equation 7 calculated the change in alveolar CO concentration during breath hold, assuming constant lung volume and uniform dilution of the inspired gas into the alveolar volume. Equation 9 calculated mean collected sample concentrations of Ne and CO using the recorded spirogram and gas diffusion equations to update lung volume and alveolar CO concentration every 30 ms. If the calculated CO concentration in the 500-ml alveolar sample (С О c) differed from the actual measured value ( С О m), then the Deo used in the diffusion equations was changed to Dco^ = Dcoo|d X [ С О J С О m + 1] X 2 where Dco^ and Dco^ are the values for Deo used in the previous and next iteration, respectively. The iterative calculation procedure started with a Deo value of 20 and iteration continued until Deo new differed from Dco(4d by less than 0.1 percent. Because gas chromatography measures wet gas concentrations, we adjusted the exhaled gas concentration to convert it to dry gas fraction, and during the calculation, all gas volumes were expressed as standard temperature and pressure, dry (STPD).
For the 3PIT method, we used the iterative search procedure as described by Graham et al. The process started with a calculation of residual volume, RV = VA — IVC + VDS. Equations 6 (inspiration), 7 (breath hold), and 9 (expiration) of Graham et al were then used to iteratively calculate Deo. In equation 6, every 30 ms the measured incremental inspired volume (obtained from the recorded spirogram) was added to the lung volume, and the added CO and Ne were used to recalculate an instantaneous value for alveolar CO and Ne concentrations using gas dilution and diffusion equations. Inspired gas concentrations were assumed to equal concentrations in the inspired gas tank, obtained by chromatography prior to the first Deo maneuver in each patient. Equation 7 calculated the change in alveolar CO concentration during breath hold, assuming constant lung volume and uniform dilution of the inspired gas into the alveolar volume. Equation 9 calculated mean collected sample concentrations of Ne and CO using the recorded spirogram and gas diffusion equations to update lung volume and alveolar CO concentration every 30 ms. If the calculated CO concentration in the 500-ml alveolar sample (С О c) differed from the actual measured value ( С О m), then the Deo used in the diffusion equations was changed to Dco^ = Dcoo|d X [ С О J С О m + 1] X 2 where Dco^ and Dco^ are the values for Deo used in the previous and next iteration, respectively. The iterative calculation procedure started with a Deo value of 20 and iteration continued until Deo new differed from Dco(4d by less than 0.1 percent. Because gas chromatography measures wet gas concentrations, we adjusted the exhaled gas concentration to convert it to dry gas fraction, and during the calculation, all gas volumes were expressed as standard temperature and pressure, dry (STPD).
Continue reading this post…
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method: Methods
Several technical abbreviations are used in the text (Table 1). Data were analyzed from diffusing capacity tests of patients referred to our outpatient pulmonary function testing laboratoiy. We did not screen the patients so that the patient population tested represents a typical sampling of patients referred to our laboratory for routine testing. The diffusing capacity was determined using an automated pulmonary function testing unit (Medical Graphics Corporation, St. Paul, Minn). When performing a test, the diffusion test gas mixture (0.3 percent CO, 0.5 percent Ne, 21 percent 02, and balance nitrogen) was first analyzed using a built-in gas chromatograph. Patients were instructed to exhale completely and then to rapidly inhale diffusion test gas and hold their breath for about 8 s. After breath hold, patients exhaled rapidly, during which the first 750 ml was discarded and the next 500 ml of expired gas was collected. In patients whose vital capacity was less than 2.0 L, the 500-ml sample was collected after 500 ml was expired. The expired gas sample was then drawn into the gas chromatograph for analysis of expired Ne and CO. Gas chromatography eliminates the need for a C02 correction.
Continue reading this post…
Comparison of Four Methods for Calculating Diffusing Capacity by the Single Breath Method
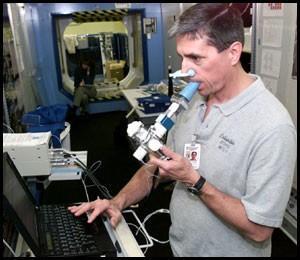 The diffusing capacity of the lungs for carbon monoxide (Deo) can be estimated by a number of techniques, including steady state, single breath, and rebreathing. The single-breath method is most commonly used in the United States, probably because of better standardization and because it does not require a rapid CO analyzer. In the singlebreath method, patients are required to take a full vital capacity breath of the test gas mixture, hold their breath for about 10 s, then exhale. The equation used for calculation of diffusing capacity has breath-hold time in the denominator, where Deo is the diffusing capacity of the lungs for carbon monoxide, Va is the alveolar volume accessible to the inhaled test gas mixture, Pb is barometric pressure in mm Hg, Fa,x and Fi,x are the alveolar and inhaled concentrations of gases (carbon monoxide, CO, or Neon, Ne), IVC is the volume of inspired gas, and Vds is the sum of system (35 ml) and anatomic (150 ml) dead spaces. The initial alveolar CO concentration (Fa,co[0]) is calculated from Fi,co times a dilution factor (equation 3). All calculations are performed with gas volumes expressed STPD, though Va is reported in BTPS for comparison with plethysmographic TLC.
The diffusing capacity of the lungs for carbon monoxide (Deo) can be estimated by a number of techniques, including steady state, single breath, and rebreathing. The single-breath method is most commonly used in the United States, probably because of better standardization and because it does not require a rapid CO analyzer. In the singlebreath method, patients are required to take a full vital capacity breath of the test gas mixture, hold their breath for about 10 s, then exhale. The equation used for calculation of diffusing capacity has breath-hold time in the denominator, where Deo is the diffusing capacity of the lungs for carbon monoxide, Va is the alveolar volume accessible to the inhaled test gas mixture, Pb is barometric pressure in mm Hg, Fa,x and Fi,x are the alveolar and inhaled concentrations of gases (carbon monoxide, CO, or Neon, Ne), IVC is the volume of inspired gas, and Vds is the sum of system (35 ml) and anatomic (150 ml) dead spaces. The initial alveolar CO concentration (Fa,co[0]) is calculated from Fi,co times a dilution factor (equation 3). All calculations are performed with gas volumes expressed STPD, though Va is reported in BTPS for comparison with plethysmographic TLC.
Implicit assumptions underlying the calculations are (1) that the alveolar surface area available for diffusion is exposed to the inhaled gas mixture for the entire time of breath hold, and (2) there is both homogeneity in delivery of inspired gas to the entire Va and homogeneity of ratios of regional Deo to Va.2 These assumptions are not strictly valid and breath-hold time becomes an approximation of the time that the test gas mixture is exposed to the exchanging surface area. canadian neighborhood pharmacy
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Conclusion
Although the strength and endurance of the inspiratory muscles improved with training, the pulmonary function parameters, especially VC and 12s-MW, did not change. Similar effects were reported by Chen and coworkers and by Flynn and associates in patients with COPD during respiratory muscle training. Pulmonary function testing is known to be an insensitive parameter of inspiratory muscle function. The 12s-MW test is influenced by many factors and it may therefore fail to distinguish inspiratory muscle dysfunction from other causes for its impairment.
In our study, training not only improved diaphragmatic and global inspiratory muscle function, but nearly all of the adaptation gained from training Was also retained 6 months after the cessation of the training. Healthy young subjects who had 4 or 5 weeks of training lost at least 50 percent of the gain after 8 to 15 weeks of no training. Belman and Gaesser have shown in normal elderly subjects that almost all the adaptations gained from 8 weeks of training were retained 2 months after its cessation. It is therefore very likely that the adaptations in ventilatory muscles become greater with increased training period.
Continue reading this post…
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Discussion
 Our study shows the following results:
Our study shows the following results:
(1) In patients with DMD, respiratory muscles and in particular the diaphragm, are trainable in terms of strength and endurance, provided that their ventilatory function is not severely restricted.
(2) In patients with VC values less than 25 percent predicted and/or a PaC02 of more than 45 mm Hg, a specific training of the inspiratory muscles does not produce any benefit. On the other hand, a damaging effect could be excluded, at least for a training period of 1 month.
The significance of skeletal muscle training in patients with neuromuscular disease is controversial. There is a scarcity of data regarding whether or not diseased muscles can be strengthened by specific training programs at all, much less the exact extent and stage of the disease at which skeletal muscles can be strengthened. In one patient with Duchenne dystrophy, histologic examination showed that those muscles assuming the least degree of sustained physical activity had the least degeneration, implying that physical activity hastened muscle fiber degeneration. It was therefore suspectpd that overwork or heavy exercise may accelerate skeletal muscle weakness in neuromuscular disease. my canadian pharmacy phone number
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Analisys
At the beginning of the study the Pesmax and Pdimax values were not significantly different in the two groups (Fig 1, Table 2). After the 6-month training period, however, the ten patients who completed the training had significantly higher Pesmax and Pdimax values than the 12 control subjects without severe functional impairment (p < 0.001) (Fig 1, Table 2). At the end of training the mean Pesmax and Pdimax values were 5.59 ± 0.98 kPa and 6.61 ±1.16 kPa, respectively, for the 10 training patients; 3.38 ± 1.18 kPa and 4.12 ± 1.11 kPa, respectively, for the 12 controls. The 12 controls without severe pulmonary function impairment, the 5 training, and the 3 control patients with severe impairment showed no significant change of Pesmax and Pdimax values during the observation period (Fig 1, Table 2). The effects of training on inspiratory muscle endurance are shown in Table 3. In the ten patients who completed the training, the endurance time increased significantly (Table 3). The reasons for terminating the test are also listed in Table 3. It should be noted that in the ten patients who completed the training, the target pressure during the resistive breathing tests increased during the training period. This means that the inspiratory task which could be sustained increased. In these ten patients, a pressure/endurance-time product was calculated by multiplying the created Pdi by Те to compare the work capacity of the inspiratory muscles before and at the end of training. The mean pressure-time product increased from 2678 kPa«s to 5500 kPa«s (p < 0.001) (Fig 2). sildenafil citrate pink
Inspiratory Muscle Training in Patients With Duchenne Muscular Dystrophy: Results
 The mean of the five highest pressure values during ten maximal static inspiratory efforts against the almost occluded airway was used as the minimal pressure value which had to be reached during such efforts at home. This value had to be adjusted each month anew, if the patients could meanwhile achieve higher mean pressure values. If a training patient showed no improvement in the inspiratory muscle function parameters after 1 month of training, he met our discontinuation criterion and was excluded from the study, since significant improvement should have occurred within 1 month. Data Analysis
The mean of the five highest pressure values during ten maximal static inspiratory efforts against the almost occluded airway was used as the minimal pressure value which had to be reached during such efforts at home. This value had to be adjusted each month anew, if the patients could meanwhile achieve higher mean pressure values. If a training patient showed no improvement in the inspiratory muscle function parameters after 1 month of training, he met our discontinuation criterion and was excluded from the study, since significant improvement should have occurred within 1 month. Data Analysis
The baseline parameters of the two groups were compared by means of the Mann-Whitney test. The changes during the training period within one group were compared by the Wilcoxon test. The Spearman rank correlation coefficient was used to test the relationship between improvement in respiratory muscle strength and endurance and baseline levels of VC. canadian neightbor pharmacy

 Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.
Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.