Latest News - Part 8
Continuous Oxygen Saturation Monitoring during Cardiac Catheterization in Adults: Angiography
When the effect of coronary cineangiography, left ventriculography, and balloon inflation during percutaneous transluminal coronary artery angioplasty on Sa02 were measured, two patients were excluded, one because he was having multiple episodes of desaturation with such frequency that we were unable to establish accurate readings for Sa02 before angiography or baseline values before angioplasty, and another because his peripheral pulses were not adequate to register accurate pulse oximeter readings during contrast injection. This population of 27 patients had 10 ±1 (range, 4 to 20) single coronary artery contrast injections per patient, with 5 to 7 ml of contrast per injection. After combining contrast injections occurring within one minute of each other into one effective injection, these 27 patients had 7 ± 1 (range, 1 to 18) effective contrast injections per patient, for a total of 182. The largest decrease in Sa02 observed within the one minute following an injection was 5 percent in one patient, and another nine injections (in eight patients) were followed by a decrease in Sa02 of 3 percent or more. Of these ten injections, in four the Sa02 decreased below 90 percent, but for no more than 12 seconds (Table 3). Continue reading this post…
Continuous Oxygen Saturation Monitoring during Cardiac Catheterization in Adults: Results
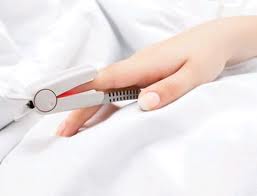 The patient population had a mean age of 53 ±3 years (range, 21 to 83 years) and mean weight of 83 ± 3 kg. Nineteen patients were men, and ten were women. Eighteen patients (62 percent) had a history of smoking. Nineteen patients received sedation before or during catheterization (14 with diazepam [2 to 15 mg], two with morphine [3 to 9 mg], and three with combinations of diazepam and morphine). The mean duration of the procedure was 96 ±5 minutes. The baseline Sa02 was 96 ±0.4 percent (range, 93 to 100 percent). All patients had a decrease in Sa02 from baseline at some time during catheterization. The lowest Sa02 for the population was 90 ± 1 percent (range, 82 to 96 percent; p<0.01 compared to baseline). Decrease from baseline to lowest Sa02 was 6 ±0.5 percent (range, 2 to 11 percent). The time at which the lowest Sa02 occurred did not relate to any event during catheterization. Continue reading this post…
The patient population had a mean age of 53 ±3 years (range, 21 to 83 years) and mean weight of 83 ± 3 kg. Nineteen patients were men, and ten were women. Eighteen patients (62 percent) had a history of smoking. Nineteen patients received sedation before or during catheterization (14 with diazepam [2 to 15 mg], two with morphine [3 to 9 mg], and three with combinations of diazepam and morphine). The mean duration of the procedure was 96 ±5 minutes. The baseline Sa02 was 96 ±0.4 percent (range, 93 to 100 percent). All patients had a decrease in Sa02 from baseline at some time during catheterization. The lowest Sa02 for the population was 90 ± 1 percent (range, 82 to 96 percent; p<0.01 compared to baseline). Decrease from baseline to lowest Sa02 was 6 ±0.5 percent (range, 2 to 11 percent). The time at which the lowest Sa02 occurred did not relate to any event during catheterization. Continue reading this post…
Continuous Oxygen Saturation Monitoring during Cardiac Catheterization in Adults: Materials and Methods
From the continuous recording of SaOa, the following data were derived for each patient: (1) lowest Sa02 persisting for at least eight seconds during the entire procedure; (2) number and duration of episodes during which Sa02 decreased below 90 percent; (3) the Sa02 immediately before and the lowest Sa02 in the one minute following ventriculography, coronary cineangiography, or balloon inflation during percutaneous transluminal coronary artery angioplasty. The patients age, sex, weight, hematocrit reading, smoking history, extent of coronary artery disease, location and extent of valvular disease, and signs of congestive heart failure before catheterization were recorded. Sedation before and during the procedure was administered at the discretion of the attending cardiologist and was recorded. actos tablets Continue reading this post…
Continuous Oxygen Saturation Monitoring during Cardiac Catheterization in Adults
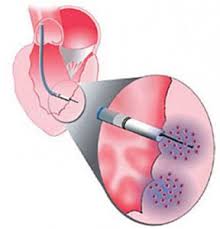 Cardiac catheterization has been associated with a variety of complications, including arrhythmias, myocardial infarction, hypotension, and acute pulmonary edema. Hypoxemia may occur during cardiac catheterization and could contribute to morbidity, as well as potentially alter physiologic parameters measured at catheterization. We know of only two published studies in which arterial hemoglobin oxygen saturation (SaOJ was continuously monitored during cardiac catheterization.* Both of those investigations were conducted on pediatric patients and were performed to determine the reliability of noninvasive Sa02 monitors. Using pulse oximetry, we examined the continuous beat-to-beat changes in Sa02 in an adult population during cardiac catheterization. Measurements of Sa02 by noninvasive pulse oximetry have been shown to be accurate over a wide range of saturations when compared to in vitro blood measurements of Sa02 using a spectrophotometric oximeter (CO-Oximeter). Continue reading this post…
Cardiac catheterization has been associated with a variety of complications, including arrhythmias, myocardial infarction, hypotension, and acute pulmonary edema. Hypoxemia may occur during cardiac catheterization and could contribute to morbidity, as well as potentially alter physiologic parameters measured at catheterization. We know of only two published studies in which arterial hemoglobin oxygen saturation (SaOJ was continuously monitored during cardiac catheterization.* Both of those investigations were conducted on pediatric patients and were performed to determine the reliability of noninvasive Sa02 monitors. Using pulse oximetry, we examined the continuous beat-to-beat changes in Sa02 in an adult population during cardiac catheterization. Measurements of Sa02 by noninvasive pulse oximetry have been shown to be accurate over a wide range of saturations when compared to in vitro blood measurements of Sa02 using a spectrophotometric oximeter (CO-Oximeter). Continue reading this post…
Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae: Summary
Excluding those patients who died, median length of stay was 2 days longer in patients who met our definition of delayed discharge. If patients were discharged within 1 day of meeting our clinical definition and receiving oral antibiotic therapy, the median length of stay for these 88 patients would have been 3 days (range, 2 to 6.75 days), with an estimated savings of approximately $507,000. These potential savings are likely underestimated given there was often a delay between IV-to-oral transition and the first day of stable clinical criteria; furthermore, we conservatively used the later day to define discharge eligibility. Our study was conducted at a single hospital, and while our patient population is likely similar to other large urban hospitals in the United States, one study has documented the distinct differences in clinical criteria used by physicians from institution to institution to determine when patients are stable for discharge, which may have influenced the impact of this variable. Additionally, clinical outcomes have not been adversely affected by decreases in length of stay (ie, discharge once patients are clinically stable without observation), suggesting that patients with CAP admitted to hospitals with historically long lengths of stay might be treated just as effectively with shorter hospital stays. It is important to note the limitations in attempting to define this variable retrospectively.
Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae: Recommendation
 The present results do confirm findings from other studies demonstrating that hospital bed costs are the major contributor to total costs for CAP. In the study by Klepser et al, room costs accounted for 34% of total hospital costs and nursing costs accounted for 37%. Although we were not able to separate nursing costs from that of room costs in our study, our hospital bed costs accounted for both direct and indirect fixed costs. When added together, the percentage of resources dedicated to room and nursing was similar with our reported hospital bed cost percentage of 55.6%. Likewise, in a separate study to assess resource utilization in the treatment of CAP, Orrick and colleagues found median costs to be $2,430 for their population, with hospital room costs constituting 83.7% of total costs, followed by antibiotic (4.6%), radiology (2.6%), and respiratory care (0.9%) costs. It is not surprising then that admission to an ICU in our study was significantly associated with an increased cost and length of stay, as daily bed cost and total length of stay (11 days vs 5 days, p < 0.001) were both greater for patients in the ICU compared with a normal hospital bed. Importantly, these data taken together confirm that antibiotic costs account for only a small percentage (< 5%) of total costs in the treatment of hospitalized patients with CAP; moreover, any efforts to reduce total or ICU length of stay, such as IV-to-oral transition or clinical pathways, will have the most profound effect on reducing the economic burden of CAP.
The present results do confirm findings from other studies demonstrating that hospital bed costs are the major contributor to total costs for CAP. In the study by Klepser et al, room costs accounted for 34% of total hospital costs and nursing costs accounted for 37%. Although we were not able to separate nursing costs from that of room costs in our study, our hospital bed costs accounted for both direct and indirect fixed costs. When added together, the percentage of resources dedicated to room and nursing was similar with our reported hospital bed cost percentage of 55.6%. Likewise, in a separate study to assess resource utilization in the treatment of CAP, Orrick and colleagues found median costs to be $2,430 for their population, with hospital room costs constituting 83.7% of total costs, followed by antibiotic (4.6%), radiology (2.6%), and respiratory care (0.9%) costs. It is not surprising then that admission to an ICU in our study was significantly associated with an increased cost and length of stay, as daily bed cost and total length of stay (11 days vs 5 days, p < 0.001) were both greater for patients in the ICU compared with a normal hospital bed. Importantly, these data taken together confirm that antibiotic costs account for only a small percentage (< 5%) of total costs in the treatment of hospitalized patients with CAP; moreover, any efforts to reduce total or ICU length of stay, such as IV-to-oral transition or clinical pathways, will have the most profound effect on reducing the economic burden of CAP.
Continue reading this post…
Resource Utilization of Adults Admitted to a Large Urban Hospital With Community-Acquired Pneumonia Caused by Streptococcus pneumoniae: Conclusion
These results conflict with other studies that have identified increased costs attributed to infection with numerous resistant organisms, including S pneumoniae. In particular, our results conflict with a retrospective, cohort study of similar size but different time period by Klepser and colleagues; these investigators evaluated health-care resource utilization for the treatment of penicillin-susceptible and penicillin-nonsusceptible isolates of S pneumoniae and found that total hospitalization costs were significantly greater for patients infected with penicillin nonsusceptible isolates ($10,309.25 vs $7,801.54, p = 0.0006). The primary reason for the higher cost was a greater length of stay among the nonsusceptible group (14 days vs 10 days, p < 0.05). Length of stay in general was much lower for patients in our study (median, 5 days) and not different between susceptible and nonsusceptible groups. It is most likely that the advances in understanding the time frame and clinical characteristics of the stable CAP patient in the current era (2000 to present) have dramatically reduced the duration of hospital stay compared with when the study by Klepser et al was conducted (1995 to 1998), therefore making it more difficult to find a difference if one were to exist. canadian neighbor pharmacy
Continue reading this post…

 Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.
Tadalafil is an orally administered drug for treating impotence (erectile dysfunction), that
initially was developed by the biotechnology company ICOS, and then developed and marketed
world-wide as Cialis, by Lilly ICOS, LLC, the joint venture of ICOS Corporation and Eli Lilly
and Company. Cialis tablets, in 5mg, 10mg, and 20mg doses, are yellow, film-coated, and
almond-shaped.